Golf Shoulder Injuries
Lennard Funk & Roger Hawkes
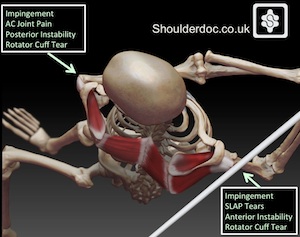
Golf is a unique sport with regards to the shoulders in that each shoulder has to do a very specific and very opposite manoeuvre in swinging the golf club. The leading shoulder is forced and stretched into an extreme adducted position at the top of the backswing and the non leading shoulder into an abducted externally rotated position. This leads to very different pathologies in each shoulder.
The leading shoulder is prone to:
- Subacromial impingement.
- AC joint pain.
- Posterior instability.
- Rotator cuff tears.
- Subacromial impingement.
- SLAP tears.
- Anterior instability.
- Rotator cuff tears.
In golf, although not being considered an overhead sport, 30% of the swing is spent vertically elevated above 90°. The combination of horizontal and vertical extremes has been shown to be a mechanism for shoulder injury particularly with the number of repetitions during play and practice (Mitchell et al. J Orth Sports Physical Therapy). Shoulder injuries are also second to spinal injuries for increasing number of rounds and balls hit per week, with a higher number of shoulder injuries in golfer’s who play four or more rounds per week or hit more than 200 hundred balls per week.
Over the years the swing has changed, with an increased torsion required by the whole trunk and shoulders in creating a powerful drive shot. This is equivalent to releasing a coiled spring. Therefore modern day golfers tend to be hyperflexible with extreme rotation between the pelvis and shoulders achieved during the swing. This is known as the X factor and a high X factor of 70° is thought to be advantageous for a powerful drive.
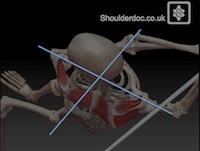
In this position the leading shoulder is in extreme adduction. This tends to lead to a shortening of the anterior shoulder structures with protraction of the shoulder. Pectoralis minor is thought to be the main protractor.
There is thought to be an equivalent lengthening/stretching of the posterior scapular muscles, particularly the rhomboids. This can be seen clinically by measuring the distance between the thoracic spine and the medial border of the scapular and comparing this to the same distance in the non leading shoulder. In extreme cases this distance will be increased showing lengthening of the rhomboids and protraction of the shoulder. Clinically a scapular dysrhythmia can also be seen with the shoulder protracting more through abduction and flexion compared to the opposite side.
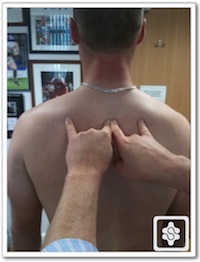
In the leading shoulder the pectoralis minor muscle becomes tight and shortened, whilst the rhomboid are stretched and lengthened:

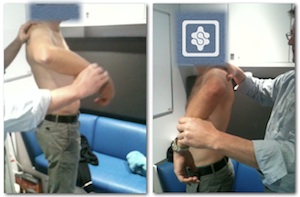
Measuring the distance from the medial border of scapula to the thoracic spine. Note the larger distance on the leading shoulder side (left):
In addition to the muscular effects above the extreme adducted position coupled with underlying joint hyerlaxity leads to excessive posterior capsular stretch and a subclinical posterior instability of the leading shoulder. This can progress to posterior labral tears as well as anterosuperior internal impingement and subacromial impingement as the greater tuberosity passes very close to the anterosuperior labrum and under the acromion. The excess posterior capsular laxity can be assessed by testing internal and external rotation in 90° abduction. One may find excess internal rotation on the leading shoulder compared to the non leading shoulder.
Posterior capsular stretch and posterior labral injury in the leading shoulder:|
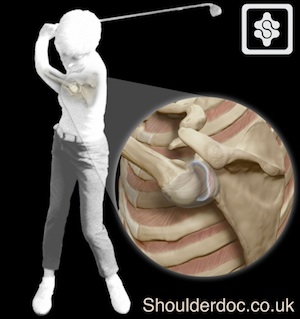
Assessment of internal rotation in the golfer. Note the excess internal rotation in the leading shoulder (left shoulder) compared to the non-leading shoulder (right shoulder):
The repetitive adducted position can also cause subacromial impingement and AC joint pain. This particularly occurs with older golfer’s who may have some pre-existing AC joint degeneration.
Internal impingement on the non-leading shoulder exists between infraspinatus and the gleno-humeral joint, due to the extreme external rotation of the golf swing.
DIAGNOSIS
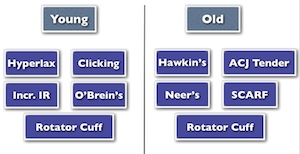
A diagnostic algorithm can be applied to both the young and the older golfer’s with a cut off age of approximately 35 years. The younger golfer’s are those that are more lax and more prone to sub clinical posterior instability, labral pathologies and secondary subacromial impingement. They may also progress to developing partial thickness rotator cuff tears.
The specific clinical findings and examination should be to assess:
- Hyperlaxity with a Beighton score.
- Painful clicking on circumduction of the shoulder.
- Excess internal rotation in abduction compared to the non leading shoulder.
- Positive O’Brien’s test with both pain and weakness particularly posteriorly as the humeral head translates posteriorly in the adducted internally rotated position.
- Subacromial impingement tests including Hawkins’ and Neer’s sign.
- Impingement tests: Hawkin's and Neer’s sign.
- Acromioclavicular joint tests: direct tenderness, Scarf test and Paxinos test, rotator cuff tests should also be performed.
INVESTIGATIONS
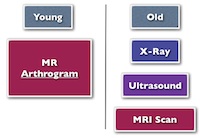
In the young patients the gold standard investigation is an MR arthrogram as this should give a better idea of the capsular laxity and labral pathologies.In the older golfer an x ray would be beneficial for AC joint pathology as well as possible impingement signs. Ultrasound scan is useful for impingement and assessing the rotator cuff and MRI scan may be useful to look for impingement from underlying osteophytes from the acromion, from the AC joint and assessing the rotator cuff as well as possible large osteochondral lesions.
MANAGEMENT
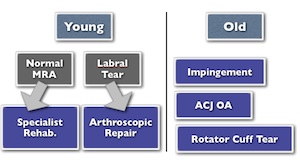
In the young golfer with a normal MR arthrogram specialist rehabilitation would be the main treatment. This should include scapular correction exercises, balancing the scapular protractors and retractors as well as sports specific rehabilitation. Core stability and working on the kinetic chain particularly for golf is essential.Should the MR arthrogram confirm a labral tear arthroscopic repair would be appropriate. However significant tightening of the posterior capsule is not recommended as this will significantly delay or restrict a return to golf.
In the older golfer the standard treatments for impingement, AC joint arthritis or rotator cuff pathology as found would apply.
Return to golf rehab post operative and post injury rehabilitation can be directed to sports specific return to golf rehab from a very early stage.
At three to four weeks following surgery or standard rehabs one handed putting with the affected arm can be started, putting through the lane by lining up shots using string instead of clubs can be done.
The swing can be recaptured and very early on by performing simple body twisting exercises reproducing the swing motions and working on core stability and kinetic chain in this way. The sport can be brought into the therapists gym by using therabands to reproduce the golf swing.
Short game strokes and ball hitting can start generally by the end of the second month with increased shoulder stretching particularly working on any tightness either anteriorly or posteriorly to return the normal golfing motion in the shoulder joint. Golf drills can generally start at the second or third month and the player return to the pre-teaching pro at that stage under guidance and with good communication from the physiotherapist and surgeon.
There should be good communication between the patient’s surgeon, physiotherapist and the teaching pro at all stages.
SUMMARY 
Shoulder injuries in golf are common. They are unique to each shoulder and also to golf. The awareness of sub clinical posterior instability in the non leading shoulder is increasing and a good multi-disciplinary treatment at all stages is the ideal management for an early return to golf.
References & Bibliography:
- Kim Mitchell, Scott A. Banks, Hiroyuki Sugaya. Shoulder Motions During the Golf Swing in Male Amateur Golfers. J Orthop Sports Phys Ther. 2003; 33(4):196-203.
- Gosheger G, Liem D, Ludwig K, Greshake O, Winkelmann W. Injuries and overuse syndromes in golf. Am J Sports Med. 2003 May-Jun;31(3):438-43.
- Smoljanovic T, Bojanic I, Hannafin JA, Hren D, Delimar D, Pecina M. Traumatic and overuse injuries among international elite junior rowers. Am J Sports Med. 2009 Jun;37(6):1193-9. Epub 2009 Mar 19.
- Hovis WD, Dean MT, Mallon WJ, Hawkins RJ. Posterior instability of the shoulder with secondary impingement in elite golfers. Am J Sports Med. 2002 Nov-Dec;30(6):886-90.
- Kim DH, Millett PJ, Warner JJ, Jobe FW. Shoulder injuries in golf. Am J Sports Med. 2004 Jul-Aug;32(5):1324-30.


