Partial Thickness Rotator Cuff Repair Technique
Partial Thickness Cuff Tears (PTCT) in athletes tend to be articular sided and typically the PASTA variant with tendon avulsion of the supraspinatus on the articular side. This is generally related to a traction injury on the arm or a traction injury sustained with dislocation or subluxation of the shoulder. Other injuries such as labral and capsular tears are not uncommonly associated with PTCT. 
There is some confusion about what constitutes a significant PTCT requiring repair. Generally it is stated that tears involving less than 50% of the tendon thickness do well with a debridement alone, yet those greater than 50% require a repair. I have found it difficult to adequately assess exactly 50% thickness in my Practice after debridement of the frayed edges of the tear. If the greater tuberosity footprint is exposed to any degree a young athlete with traumatic to their shoulder I would proceed to an arthroscopic repair. 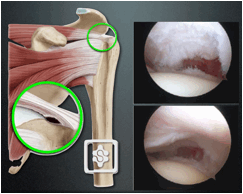
PRE-OPERATIVE SYMPTOMS
Pre-operative symptoms suggestive of a PTCT are a positive Jobes resisted supraspinatus test, positive empty can or full can test with pain and or weakness. Impingement tests are not always positive and should they be present a subacromial decompression is considered.
IMAGING INVESTIGATIONS
Imaging investigations involve an ultrasound scan which is dependent on the operator and quality of the ultrasound machine. On a good quality modern machine there should be an over 80% sensitivity for significant PTCT.
MR Arthrogram is beneficial, particularly in athletes where there are associated labral pathologies on the ABER view. Detachment of the articular side of the supraspinatus can often be seen and associated labral tears can be seen.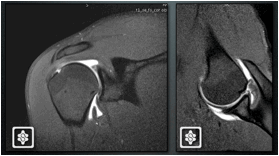
INCIDENCE
The incidence of PTCT is low. I reviewed my Practice between 2005 and 2010 (5 years) there were 3,234 shoulder operations, 539 of those were on elite competitive athletes (18%). In total there were 21 PTCT repairs and 47 debridements. 14 of the 21 PTCT repairs were in elite athletes (67%). Of these there were 8 rugby, 2 cricket, 1 javelin, 1 tennis, 1 bobsleigh, 1 paralympic tennis. Therefore, in total only 0.7% of all shoulder operations in a busy specialist shoulder service with an interest in sports injuries were PTCT repairs!
TECHNIQUE
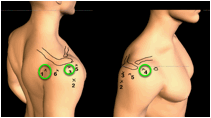 | Portals: The posterior, anterior and superolateral portals are the only portals required. |
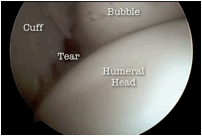 | Looking from the glenohumeral side a bubble may often be seen under the rotator cuff. This is suggestive that the tear is not full thickness. |
 | The frayed edges of the tear are then debrided via the anterior portal
and the thickness of the tear can then be assessed. If the footprint is
then exposed a repair is then undertaken in the young athletic patient. |
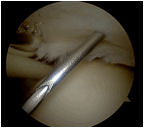 | The medial edge of the tear is marked via the glenohumeral joint using a needle and a No.1 PDS suture is passed through the needle. |
 | The scope is then inserted into the subacromial bursa via the posterior
portal. The PDS suture can then be seen in the bursa and the rotator
cuff lateral to the PDS suture is then probed. If this very thin and
the probe easily falls through the tissue here the tear is then
completed and the tear repaired as a full thickness rotator cuff repair
via the bursal side. However if the rotator cuff is probed and the
tendon quality is felt to be thick and good quality a trans-tendinous
parachute repair is then undertaken. The bursa is cleared sufficiently to allow knot tying in the bursa later in the procedure. |
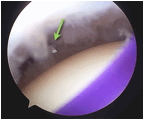 | The scope is then inserted back into the glenohumeral joint via the
posterior portal. The PTCT is then opened with a No.11 knife blade in
the line of the supraspinatus tendon fibres and a soft tissue shaver
inserted to debride the footprint area further. |
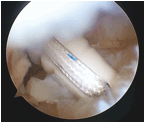 | A 5mm double or triple loaded suture anchor is then inserted into the greater tuberosity trans-tendinous. Using a suture manipulator the sutures are retrieved into the joint partially via the anterior portal to allow easy capture of the sutures in the next step. |
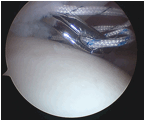 | A suture grasper curved and pointed (such as Cleverhook, Mitek DePuy; Rhino, Arthrex Ltd; Arthropierce curved, Smith & Nephew) is inserted through the good tissue of the rotator cuff just medial to the tear. Each suture limb from the anchor is taken through a separate hole with 2 same colour suture limbs taken medially and the other colour suture limbs taken more laterally. |
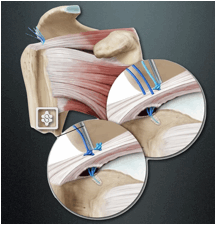 | The same colour suture limbs are tied via the bursal side and the repair thus completed. A subacromial decompression is added should the patient has suffered with impingement features pre-operatively. |
Post-operatively for athletes we use a tailored rehabilitation protocol as developed by our Shoulder Team in conjunction with Rugby Club Physiotherapists. The approach is player specific to suit the players age, position requirements, as well as the Surgeon and Therapist. The rehab protocol is not an accelerated or aggressive or time specific. The protocol is a guide and not a prescription. Communication between the Player, Therapist and Training Staff is essential throughout the rehabilitation programme. Progression to each phase is when the patient is able to perform all of the exercises in the previous phase without any discomfort or apprehension. Each phase is introduced progressively.


