Decompression of the Suprascapular Nerve
Compression of the suprascapular nerve may be as a result of injury, swelling secondary to scapular fractures, or an idiopathic nerve compression presumed secondary to local swelling, rather analogous to carpal tunnel syndrome. It may be secondarily compressed because of local lesions such as neuroma or ganglia or anomalies of the suprascapular notch itself.
Indications
Patients present with weakness of external rotation and no sensory loss, but visible wasting of supraspinatus and infraspinatus may be evident. Patients complain of a dull aching pain and characteristically grasp their suprascapular area -with the opposite hand.
Preoperative Investigation
The prime investigation is an electromyographic study to confirm a block in the nerve. Because of wasting of supraspinatus and infraspinatus and the loss of function, it may well be confused with a rotator cuff tear. Therefore, shoulder arthrography, magnetic resonance imaging, or arthroscopy may be needed to elucidate this. Computed tomography may be helpful in identifying the area of nerve compression itself, and localized ganglia may be seen by ultrasound scanning alone.
Position of Patient
The lateral position is used with the involved extremity uppermost and draped separately to allow rotation.
Technique
The most common site for the nerve to be compressed is at the suprascapular notch. The nerve may be decompressed by excising the transverse suprascapular ligament and freeing the nerve at this site.
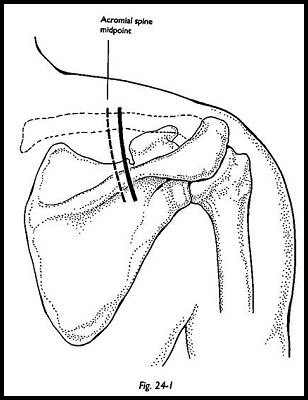
A vertical incision is made centered on a point on the acromial spine, just lateral to the midpoint from the medial border of the scapula to the lateral point of the acromion (Fig. 24-1). The vertical incision extends across the supraspinous fossa.
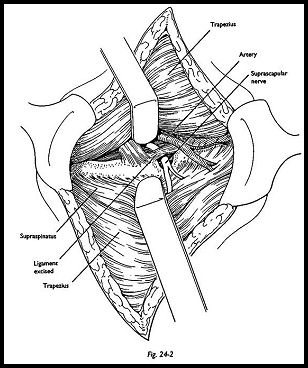
Skin and subcutaneous tissue is incised, and the fibers of the trapezius are identified and split in the line of the fibers in the lateral part of the wound by blunt dissection. The underlying supraspinatus muscle is now visible, and the supraspinatus notch is palpated anterior to the supraspinatus muscle. The supraspinatus muscle is mobilized and retracted inferiorly. This is a surprisingly deep wound; a head light or an illuminated retractor is helpful. The artery is seen to cross superficial to the ligament and the nerve deep to it (Fig. 24-2). The artery is bluntly dissected to one side, and the ligament is excised. The suprascapular notch is inspected. If there is any bony encroachment on the nerve, the notch can be enlarged with small bone nibblers. Sometimes only infraspinatus may be affected, and hence the compression may be more distal. By retracting the supraspinatus muscle superiorly, one can inspect the nerve further distally at the spinoglenoid notch. Occasionally, compression may be caused here by the spinoglenoid ligament, but this is not often present. If the ligament is found and thought to be causing compression, it can be excised. The wound is closed in layers without drainage.
Postoperative Management
A sling is worn for comfort only. Gentle mobilizing exercises are begun the day after surgery as pain allows. The arm is mobilized actively within pain limits to allow for soft tissue healing.
Suggested Readings
Miniaci A, Tibone JE: Suprascapular neuropathy, pp. 103-5. In Paulos LE, Tibone JE (eds): Operative Techniques in Shoulder Surgery. Aspen Publishers, Aspen, CO, 1991
Vastamaki M: Diagnosis and management of suprascapular nerve entrapment. Proceedings of Third International Conference on Surgery of the Shoulder for Kyoko of Japan 1986. National Postgraduate Services, Tokyo, 1987


