SLAP Tear Management
Lennard Funk, 2010
In this article we will discuss the superior labrum, what is a SLAP tear, the approach to each type of SLAP tear and some of the results of SLAP repairs.
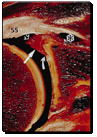 If we look at the superior labral complex it is totally adherent to the superior glenoid and congruent with the articular cartilage of the glenoid. The superior labrum may have a meniscoid variant but within the meniscoid variant the articular cartilage is still not undercut and the superior labrum is still tightly adherent to the superior glenoid bone.
If we look at the superior labral complex it is totally adherent to the superior glenoid and congruent with the articular cartilage of the glenoid. The superior labrum may have a meniscoid variant but within the meniscoid variant the articular cartilage is still not undercut and the superior labrum is still tightly adherent to the superior glenoid bone.
The blood supply of the superior glenoid and labrum is predominantly from the long head of biceps and to a much smaller extent from the glenoid bone. There is a watershed area in the anterior superior labrum which creates a potential for tears and also maybe significant with regards to the healing of SLAP tears in older patients and chronic tears (Peters, 1992; Guttmann, 2010).
INDICATIONS FOR SURGERY
The indications to proceed to an arthroscopy and probable SLAP repair would not be based on any one particular finding. I use a combination of the history, clinical examination and findings on MR Arthrogram. Within the history patients are generally athletes with a specific traumatic event consistent with a SLAP tear. This may be a throwing injury with a peel back mechanism or a direct impact landing on the elbow with the shoulder flexed forcing the humeral head up and avulsing the superior labrum or a traction injury on the superior labrum, such as that sustained in a dislocation or a subluxation of the shoulder joint. The patient will also have some typical symptoms consistent with a SLAP tear, such as painful clicking and clunking from the joint, possible locking, pain on eccentrically loading the biceps such as pulling through the water in a swimmer, on making contact with a ball in racquet sports and on releasing the ball in throwing.
There is no single good clinical examination test for a SLAP tear and therefore a combination of tests is preferred. My preference is a combination of the OBriens test, Kibler clunk test and a labral load test.
MR Arthrogram findings consistent with a SLAP tear would also further support the diagnosis, however the accuracy on MR Arthrogram is 75% to 90%, bearing in mind that a SLAP tear is a dynamic injury and an MR Arthrogram a static investigation. A number of smaller tests may be missed on MR Arthrogram. A Shoulder Surgeon should also review the scan images themselves and reporting of MR Artghrograms is dependent on the definition used by the Radiologist for a SLAP tear since these differ in the radiological literature.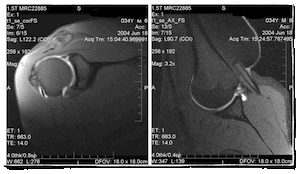
ARTHROSCOPY
At arthroscopy there may be some disagreement as to what constitutes a true SLAP tear. This would be a combination of the clinical findings and history above but a true SLAP tear also is one which can be lifted beyond the articular cartilage at the superior glenoid exposing the bone of the superior glenoid neck. This area should not be visible when lifting the superior labrum in an intact superior labrum. This definition was described in the 1980s by Andrews and Snyder.
MANAGEMENT BY TEAR TYPE
SLAP I TEAR
SLAP I tears are rare and more commonly found in older degenerative patients. These do not require a repair and may be treated with debridement alone.
SLAP II IV TEARS
These SLAP tears constitute a detachment of the superior labrum and require surgical fixation. Looking at the incidence of SLAP repairs in my Practice over a 10 month period from January to October 2010 we undertook 27 SLAP repairs. The vast majority of these were SLAP Type II (C) tears involving the anterior posterior footprints, followed by SLAP II (B) tears. 88% of these injuries were sports related and the average age was young at 26.3 years (range 18 to 47). The majority were males with a ratio of male to female of 21 to 6. The commonest sport involved was rugby.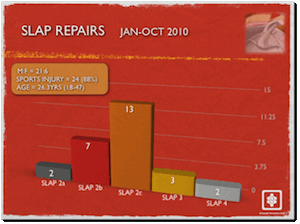
SLAP II (B) REPAIR
Note: A detachment of the posterior superior labrum may be associated with posterior labral tear and therefore the posterior labrum should always be viewed via the anterior portal as well.
 | 1. Viewing from the posterior portal a cannula is inserted through the rotator interval and the superior glenoid debrided with a bone shaver. |
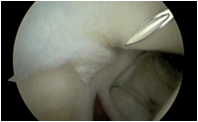 | 2. A trans-tendinous portal is created through the supraspinatus rotator cuff musculotendinous region behind the long head of biceps and just lateral to the acromion using an outside in technique with a needle and a No. 11 blade is inserted to make a small longitudinal split in the cuff. |
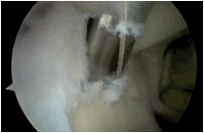 | 3. A small suture anchor cannula inserted, a hole drilled and a double loaded high strength suture anchor is inserted. |
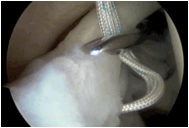 | 4. A 45 degree suture hook is inserted via the anterior portal. For a right shoulder a left sided suture hook is used and for a left shoulder a right sided suture anchor is used. This is passed underneath the long head of biceps over the top of the postero superior labrum and passed through the postero superior labrum. It is important to avoid catching any of the superior capsule or supraspinatus muscle with the suture hook. |
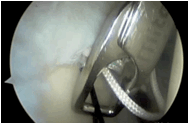 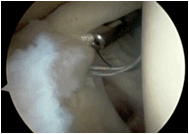 | 5. The sutures are then taken through the anterior cannula and with good suture management the suture is then tied. The labrum is assessed for stability . Often the second suture is required posterior to the long head of biceps origin as well. The repair should be assessed for stability via the anterior and also posterior portals. |
There has been concern about the trans-rotator cuff portal, however in a study in The American Journal of Sports Medicine in May 2008 by Han Oh et al this portal was shown to be safe both clinically and on CT Arthrograms over 6 months post operatively.
SLAP TYPE II (C)
Click here for animation of the technique
SLAP TYPE II (A) TEAR
For Type II (A) tears a single anterior portal can be used with a crescent suture hook as for the anterior repair of a type II (C) tear above.
SLAP TYPE III TEAR
Type III SLAP tears involve a bucket handle tear of the superior labrum. The bucket handle should be excised via the anterior portal. It may be necessary to swap portals and remove any fragments of the posterior labrum. It is also essential to assess the anterior and posterior labrums for associated tears. The remaining superior labrum should then be assessed for stability. Should there be a detachment here this can be repaired as for a Type II(C) SLAP repair above, or if this is stable it can be left alone.
SLAP IV REPAIRS
SLAP IV tears involve labral detachment extending into the long head of biceps. These tears can be repaired if the tear is fresh and healthy and the patient is young. However in more chronic tear in an older patient the detached labrum can be excised and a long head of biceps tenodesis performed. My preference is for an extra-articular biceps tenodesis with an Interference screw in these situations.
RESULTS
We published our results in The Clinical Journal of Sports Medicine in 2006 on rugby players (Snow & Funk, CJSM 2006). There was a high satisfactory at 3 to 6 months with a return to play of 89% at 3 months and 94% at 6 months.
Friel et al, JSES September 2010 published longer term results in all comers including athletes and non-athletes. This was a 3.4 year follow up of 48 cases with an average age of 33 years. There was no difference between athletes and non-athletes and a 54% return to previous level of sport. The patients in this study were all repetitive overhead athletes, predominantly baseball and some tennis. Baseball players fared better than the tennis players.
If one looks at the return to sports after SLAP repairs there is great variation in the literature. On deeper inspection it would appear that the variation in return to sports is related to the patient groups. In the studies which varied significantly the repetitive overhead and throwing athletes had a lower incidence of return to sports than the non-overhead and throwing athletes. There was also a difference in age groups with younger patients having a higher likelihood of return to sports than older patients. This is to be expected as the pathology in a repetitive chronic overhead throwing athletes shoulder is multi-factorial with elements of posterior capsular tightness, rotator cuff involvement and muscle imbalance problems. Whereas a single traumatic event in a non-overhead throwing athlete is more likely to do better since they have less chronic problems. See table below.
SUMMARY
In this article we have reviewed the indications, techniques and results for SLAP repairs. In athletes SLAP repairs do appear to be effective. SLAP tears can be diagnosed using a combination of symptoms, signs and MR Arthrography. The technique for repair is specific for the tear pattern and associated pathologies should also be looked for and addressed. The results of SLAP repairs in non-overhead athletes tend to be better than repetitive overhead throwing athletes.


