Shoulder Impingement in Athletes
Lennard Funk
Subacromial impingement has traditionally been defined as the mechanical compression of subacromial structures between the coracoacromial arch and the humerus during active elevation of the arm above shoulder level. Recent evidence and an improved understanding of the biomechanical processes causing the impingement pain and has shown us that the process is probably multi-factorial and not just caused by an acromial spur. This is particularly true in athletes.
Causes:
The cause of impingement can be as either functional or structural.
Structural is a narrowing of the subacromial space by space-occupying structures, such as an acromial spur, arthritic acromioclavicular joint or calcific deposit. It occurs in middle age.
Functional is much more common in younger athletes and is due to an injury in the glenohumeral joint (labral or capsular tear) or muscular imbalances of repetitive overhead sports.
Diagnosis:
The classical history is a gradual onset of lateral upper arm pain with overhead activities. It may follow an injury or repetitive overhead sports. Patients classically have pain on arm elevation in the mid arc range. The classical examination tests for impingement include Hawkins’ test and Neer’s sign have been shown to have high sensitivity, but low specificity.
Determining the cause of impingement will depend on the athlete’s age and their sport.
Young Overhead Athlete:
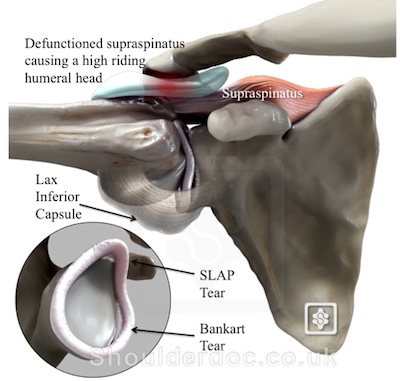
- In the younger patient (approximately less than thirty years of age) repetitive overhead activities lead to imbalance of the shoulder capsule with relative tightening and contracture posteriorly and relative stretching of the anterior capsular structures.
- Along with this there is a muscular imbalance between the eccentric and concentric throwing muscles of the shoulder. These patients often develop muscular fatigue of their supporting scapular muscles which in addition to the abnormally translated humeral head leads to poor excursion of the scapular upwards with hyperabduction of the arm leading to a narrowing of the acromiohumeral gap.
- With the abnormal posterior translation of the humeral head and capsular imbalance with poor mobility of the scapular the humeral head can impinge against the posterior glenoid entrapping the rotator cuff leading to a condition known as internal impingement, i.e. an impingement within the glenohumeral joint as well as subacromial impingement.
- It often can be difficult to clinically discern between the two and they are often coexistent in the chronic overhead athletes shoulder.
- They are often very well muscled and at risk of sustaining more traumatic injuries to their shoulder.
- The commonest structures injured here in the absence of a true shoulder dislocation are labral injuries. This is not uncommon in rugby players and is known as sub-clinical instability or microinstability.
- The sub-clinical instability of the glenohumeral joint leads to rotator cuff dysfunction. In so doing the rotator cuff is not able to contain the humeral head in abduction leading to superior translation of the humeral head with arm elevation thus subacromial impingement and subsequent bursitis.
- Simply treating the impingement will not lead to a cure unless the underlying cause and functional abnormalities are addressed in these young patients.
Older patients:
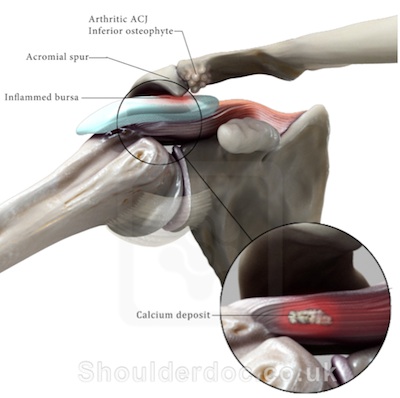
- Over the age of approximately 35 the impingement tends to be more degenerative in nature.
- Impingement and narrowing of the bursa could be due to acromioclavicular joint arthritis with inferior osteophytes impinging against the rotator cuff in abduction.
- The concept of a subacromial spur is well recognised and this can also narrow the acromiohumeral gap leading to a higher risk of impingement.
- Rotator cuff degeneration or tears leads to cuff dysfunction with poor containment of the humeral head against the glenoid in abduction, superior translation and impingement.
- It is likely that a combination of the above three factors co-exist causing impingement, i.e. a natural degenerative narrowing the acromiohumeral gap complicated by tendon degeneration and/or partial or full thickness rotator cuff tears.
Investigations
This will depend on the patient’s age. In younger patients the aetiology is most likely due to a degree of instability or internal impingement. The investigation of choice is MR-Arthrogram which will reveal any capsular ligamentous abnormalities as well as any possible partial cuff tears.
In the older athlete a plain x-ray may reveal a narrow acromiohumeral gap due to acromioclavicular osteophytes or spurs. It will also reveal any possible calcific tendonitis of the rotator cuff. Ultrasound scan is also beneficial and convenient to reveal any partial or full thickness rotator cuff tears. A plain MR scan is the investigation of choice, which will show all of the above along with any inflammatory changes if the correct MR sequences are performed.
Management
- Relative Rest: A period of relative rest involves avoiding the abusive loads and reducing speed of movement. The athlete should refrain from exercises and training that aggravate the shoulder.
- Physiotherapy: This should involve addressing the muscles and correct movements of the scapular, core stability, postural rehabilitation, address rotator cuff imbalances and posterior capsular tightness if present. The physiotherapy exercises should not reproduce the impingement pain.
For the athlete we would recommend two to three months on this programme with gradual re-introduction of specific sports exercises as tolerated. - Corticosteroid Injection: The role of a subacromial corticosteroid injection is to alleviate the bursal inflammation to allow the rehabilitative processes to continue if pain and inflammation was not adequately controlled with non-steroidal anti-inflammatories and analgesics alone.
- Referral to Shoulder Specialist: Should there be a failure to improve with the above programme referral to a specialist shoulder surgeon is advised where imaging investigations as above can be performed and surgical intervention undertaken if necessary. The surgery for a younger patient would involve a capsular labral repair with or without a subacromial decompression depending on the MR arthrogram and findings at surgery. For a more mature athlete a subacromial decompression, acromioclavicular joint excision and rotator cuff repair or debridement are the most common procedures. Again this will depend on the findings on the x rays, ultrasound scans and MRI scans as appropriate and surgical findings.
- Young patients with impingement consider sub clinical instability with possible capsule and labral pathology. Scapular muscle problems are also common.
- Older athletes causes are often degenerate and related to acromial spur, AC joint arthritis and rotator cuff tendonopathy or tears.
- Treatment initially involves relative rest and specific targeted rehabilitation addressing all issues including posture, scapular, rotator cuff and core stability. MR arthrogram is preferred in younger patients. X ray, ultrasound and MRI scan is preferred in older patients.
- Corticosteroid injections are an aid to the rehabilitation addressing the bursitis.
- Surgery is indicated where two to three months of appropriate and sports specific rehabilitation has failed.
- Surgery in the younger patient involves capsular labral reconstruction with or without subacromial decompression. Surgery in the older patient involves subacromial decompression with or without acromioclavicular joint excision and rotator cuff debridement or repair.
References:
- Hawkins, Kennedy. Impingement Syndromes in Athletes. AJSM, 1980
- Michener LA, Walsworth MK, Burnet EN. Effectiveness of rehabilitation for patients with subacromial impingement syndrome: a systematic review. J Hand Ther. 2004 Apr-Jun;17(2):152-64.
- JS Lewis, AS Green, S Dekel. The aetiology of subacromial impingement syndrome. Physiotherapy, 2001
- H Ellman, SP Kay. Arthroscopic subacromial decompression for chronic impingement. Two-to five-year results. Journal of Bone & Joint Surgery, British. 1991
Also See:


