Equipment
For diagnostic shoulder arthroscopy
A standard 30 degree knee arthroscope is used for shoulder arthroscopy. The shoulder is a large joint and we have found that a small diameter arthroscope gives too small a picture of the joint, as well as having difficulty delivering enough light to illuminate the far recesses of the joint cavity. Obviously a good light source and either sterile saline or Hartmann's solution is required along with the arthroscope. The only other piece of equipment needed is a wide-bore needle to establish an outflow, and a hook probe.
For arthroscopic surgery of the shoulder
Basics
For simple surgery, such as the removal of loose bodies and synovial biopsies, the only equipment needed are the standard arthroscopic tools of the trade as used for knee surgery, in particular a pair of arthroscopic grasping forceps, basket forceps and small pituitary rongeurs (Figure 4.2).
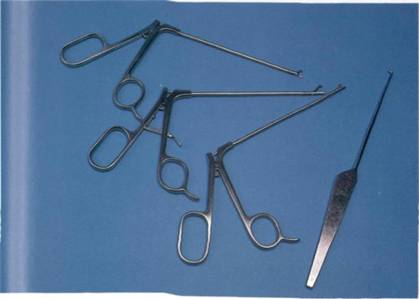
Figure 4.2 Basic instruments: from left, scissors, graspers, basket forceps, and hook probe.
Television system
For any form of more complex surgery, a television system is mandatory. Again any system that works for the knee will work for the shoulder. There have been rapid advances in camera technology recently and, in buying a camera system, the minimal requirements are a lightweight balanced camera head capable of repeated immersion for sterilization, with a white set memory to establish colour balance, allied to a high intensity light source and high resolution colour monitor.
If the shoulder is being arthroscoped in the normal lateral position, then the television monitor should be placed opposite the surgeon, the centre of the screen being on a level with the surgeon's eye. One problem that arises in shoulder arthroscopy is that if the arthroscope is changed from the routine posterior portal to the anterior portal, the surgeon can feel awkward still looking forward at the monitor in front of him. Body image becomes distorted and triangulation difficult, similar to attempting to perform internal fixation of a femoral neck fracture under image intensifier control with the intensifier image upside down and back to front. The dedicated arthroscopist will have a second monitor stationed behind him and, when he changes to the anterior portal, he then looks over his shoulder at the second monitor, or moves to the other side of the operating table and looks at the second monitor, in order to overcome 'body image' problems.
Once a good television system has been purchased, it costs little more to link a video recorder into the system to get a permanent record of the procedures. For the surgeon who has everything, this system can be linked to printers and recorders which can store images on computer disk, or reproduce them as slides, prints, transparencies, or videotape recordings. A character generator can also be used to identify each recording.
Whereas a large amount of arthroscopic surgery of the knee can be performed with hand-operated instruments, arthroscopic surgery of the shoulder really requires powered instrumentation. Powered systems mean that there is less need for instruments to be passed in and out of the joint, for, with most of these systems, the excised tissue is sucked out of the joint down the shaver or bur shaft. This is important, as the shoulder is surrounded by a greater mass of soft tissue than the knee, making entry more difficult and more traumatic to the tissues. The fewer times a portal is transgressed, the better for the shoulder.
Arthroscopic subacromial decompression can be performed with a powered soft tissue resector and powered burs alone (see Chapter 8). However, the amount of bleeding, and therefore the time taken to complete the procedure, is reduced if an electrosurgical apparatus is used to define the area of resection and cut the soft tissue off the undersurface of the acromion first (Figure 4.3).
Shoulder repair is dependent upon very specialized equipment, and the choice depends upon the surgeon's philosophy regarding method of repair (see Chapter 7). For staple repair, Instrument Makar staples are needed (Figure 4.4); for the Caspari-type repair, the Caspari punch is needed (Figure 4.5) and, for the Morgan suture technique, Bowen needles are required (Figure 4.6). Many new techniques are being developed and there is no doubt that these will require specialized instruments of their own.


Figure 4.3 Electrosurgical apparatus is useful for subacromial decompression.
Figure 4.4 The Instrument Makar arthroscopic staple.
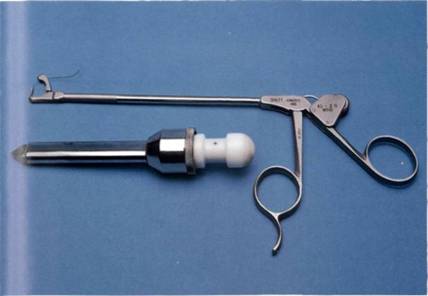
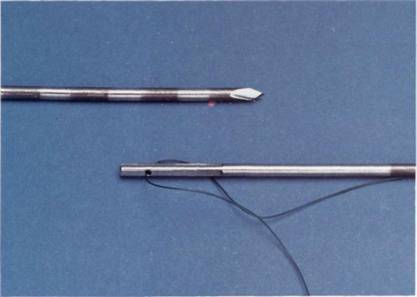
Figure 4.5 The Caspari suture punch for suture repair.
Figure 4.6 Bowen needles for suture repair.


