The pathology of the subacromial bursa and...
CHAPTER III
THE PATHOLOGY OF THE SUBACROMIAL BURSA AND OF THE SUPRASPINATUS TENDON
I DO NOT propose to review in detail the pathology of such general conditions as tuberculosis and syphilis, which, of course, may occur in this region, but merely to attempt to describe such pathologic changes as I have myself seen at operation in about two hundred explorations of the bursa on living patients. I have kept no record of the number of times I have studied the bursa in the cadaver, but I am sure I have opened over five hundred subacromial bursae, perhaps a thousand. It is significant that most of the pathological changes which I have noted had not been previously described, at least, so far as this particular bursa is concerned; and, per contra, the conventional pathologic conditions, such as suppurative inflammation, "rheumatic changes," syphilis, tuberculosis, new growths, etc., have seldom been observed by me. In the shoulder these lesions are relatively rare. On the other hand, lesions peculiar to this region are so often present that I have observed some of them in probably one-third of all the bursae I have examined in the dead, and, of course, in nearly all of the living cases. Fortunately, within the last few years, I have had the privilege of studying a much more systematic series of observations made by Dr. I. B. Akerson of the pathologic staff of the Harvard Medical School and pathologist to the Long Island Hospital of the Institutions Department of the City of Boston. We have published together in the Annals of Surgery for January, 1931, an article on "The Pathology Associated with Rupture of the Supraspinatus Tendon." The following quotation is from this paper:
"The present study has been made from autopsy material obtained at a large municipal hospital for chronic conditions. The patients sent to this hospital are people who are aged and down-and-out, and owing to the chronic character of their diseases, cannot be cared for at the other Boston hospitals. Dr. Akerson has made a study from one hundred specimens taken from fifty-two consecutive autopsies, and the percentage of cases showing evidence that the supraspinatus tendon had been ruptured at some time during the lives of these patients is high—39%. It may, therefore, be taken as a maximum, and it may be expected that pathologists performing routine autopsies in general hospitals for acute diseases, where the ages average considerably younger, will find a decidedly smaller percentage. We have made no attempt to correlate the past histories of these patients as to trauma or occupation with the autopsy findings. It would have been hardly possible under the circumstances.
"As a routine method of examination of these cases, we recommend the pathologist to employ the form of incision which we use in operations on the living. A cut is made on the anterior aspect of the shoulder joint from the acromio-clavicular articulation downward for about two inches. The fibers of the deltoid are separated and retracted and the roof of the bursa is incised between two pairs of forceps as one opens the peritoneum. When the lips of the wound are retracted, the surface of the floor of the bursa can be made to pass in review by rotating the humerus. The base of the normal bursa is smooth and spherical and almost as colorless as the cartilaginous surface of the head of the bone, though it lacks the bluish luster of cartilage. Most rents in the tendons of the short rotators usually appear in this base as communications directly into the joint and are readily visible. Occasionally the tendon is ruptured beneath the base of the bursa, which is left intact. In the ordinary autopsy it would take but a few minutes' extra time to examine both bursa. If lesions are found, the head of the bone with the insertions of the short rotators can be removed and studied. This was the method used by Dr. Akerson and his findings are good evidence that some sort of pathological process has been at work in the subacromial bursae of these patients during their lifetime. One must understand that these findings are those accumulated by each individual subject in many years. They are end-results, not acute lesions."
Dr. Akerson has continued his observations and at the present date (January, 1933) has recorded his findings on 200 shoulder joints in 102 subjects. I am greatly indebted to him for the opportunity of studying this material and the many microscopic sections he has made from it.
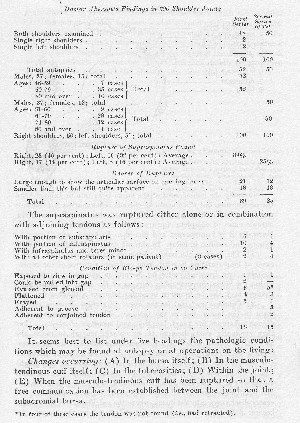

It seems best to list under five headings the pathologic conditions which may be found at autopsy or at operations on the living:
Changes occurring: (A) In the bursa itself; (B) In the musculotendinous cuff itself; (C) In the tuberosities; (D) Within the joint; (E) When the musculo-tendinous cuff has been ruptured so that a free communication has been established between the joint and the subacromial bursa.
*In four of these cases the tendon was not found (i.e., had retracted).
A. CHANGES WITHIN BURSA
.jpg)
Normally the incised roof of the bursa is as thin or thinner than the peritoneum,- but when acute or chronic inflammation is present it may be as thick as blotting paper. It is apt to be especially firm in old, chronic cases of complete rupture of the cuff, when fluid is present. Normally it is transparent and film-like. In acute cases it may be opaque and reddish in color. In chronic cases it is whitish and firm.
(1) The roof of the bursa seldom shows any pathology, but in cases of long-standing bursitis from complete rupture of the supra-spinatus, one frequently sees by X-ray, or one can palpate from within the bursa, hypertrophic changes at the acromial edge. Such changes may also be found in muscular laborers without symptoms.
(2) Calcified material in the bursa. Calcified deposits do not form in the bursa, but in the tendons. They may remain in the tendon substance for years, but the usual sequence of events is that they gradually work through to, or enlarge enough to reach, the base of the bursa, where they produce a mound-like swelling resembling a little boil, with a white center and a turgid zone about it. Up to this time there may have been no symptoms or very slight ones. Then some slight accident or unusual effort or even some customary action, as in turning over in bed, causes tension in the tendon resulting in rupture of a few superficial fibers, so that the little crater discharges into the bursa, where the calcified particles at once become diffused and may be readily delineated by the X-ray. An acute bursitis is produced; fluid is secreted with which the calcified particles mingle; fibrin appears and the specks of calcium become entangled in it. I have several times operated at this stage within a few days of the perforation and removed from the bursa a delicate film of fibrin shaped like a watch glass. Grossly the film is whitish in color and the microscope shows calcified particles scattered throughout its substance like stars in the sky.
.jpg)
FIGURE 34. PEFORATION INTO BURSA
Diagrammatic illustration of a calcified deposit bursting into the subacromial bursa. This should be compared with Fig. 4 in Plate II, which was taken from the case alluded to below.
Soon after the material is thus forced into the bursa and becomes enmeshed in fibrin, the particles are rapidly eliminated, probably by the prompt action of leucocytes. This is not the case while they still remain in the tendon. When the operation on these cases was within a few days of the perforation, I have been able to readily remove the film of fibrin almost intact, but in one case, on the sixth day after perforation, I found the film so firmly adherent that no attempt was made to remove it, because I should have had to use a curette and feared that I might destroy the membrane and get obstinate adhesions in its place. Through the kindness of Dr. H. F. R. Watts, who followed the patient with weekly X-ray pictures, I found that absorption of all the calcified material took place within three weeks of the perforation. The patient was then free from symptoms. I was encouraged in making this decision in this case by the fact that I had previously had a number of cases in which rapid disappearance of the particles had taken place without any operation. I now feel that perforation is nature's method of getting rid of this condition and that the average case, where perforation into the bursa has occurred, if left entirely to nature without any treatment, would follow this course. I think this fact accounts for the encouraging results sometimes obtained by all sorts of treatment, whether diathermy, foreign proteids, alpine lamp or surgery. This favorable course is not always the outcome, however. The inflammatory reaction may be too intense, and adhesions and consequent "frozen shoulder" result. It may be months before the adhesions loosen and full motion returns. Sometimes the whole deposit is not discharged into the bursa and the residue may give trouble later.
Under this heading we have discussed only the bursitis caused by the perforation of the calcareous material into the bursa. The study of the deposits themselves will be taken up again under Section B.
(3) Defects in the base of the bursa. These defects are nearly always at the same critical point, almost in the center of the base, where the red zones, calcified deposits and "straps" occur. The description of these defects properly belongs under the next division of our subject, for they consist of lesions of the tendon itself, whether partial or complete. Should the reader undertake to verify my statements by observing the conditions found by incising the bursa in a series of autopsies, he will be surprised at first by the variety of appearances which tears in the tendons may cause. After he has seen the inside of fifty or a hundred bursae, the secondary appearances due to the synovitis set up by the lesion will cease to distract him and his surprise will then consist in seeing how much alike the fundamental lesions are.
In other words, the superficial appearances of these defects vary with the extent of the rupture, the amount of joint cartilage exposed through the rent, the position of the lesions, the proliferation of the adjacent membrane, the extent of exposure of the biceps tendon, the degree of involvement of the adjacent tendons, the duration since the accident, the extent of formation of a falciform edge, the amount of recession or hypertrophy of the tuberosity, etc. Yet after sufficient experience, rupture of the tendon of the supraspinatus will be seen to be the basis of almost all the lesions. His chief doubt will be as to whether degeneration of the tendon always precedes rupture, although he will be convinced that rupture has certainly occurred whether the tendon was previously sound or senile in texture.
(4) Synovial villi. These are the most common evidence of pathology one encounters in the bursa itself. It is difficult to say that a given degree of roughening of the serosa is abnormal. Is callus on the palm pathologic? It may be that in the same way some
of these villi represent overuse rather than inflammation. On opening the bursa one sees strands of filmy tissue crossing the space after the air has been let in. Sometimes instead of being attached at their ends to both floor and ceiling, one end will be free so that the capillary villous will drift about in the bursa. In such cases the whole floor of the bursa is apt to be velvety with lesser villi and thickened nictitating folds. The center of this process is usually over the attachment of the supraspinatus to the tuberosity. In fact, this point seems to be the locus minoris resistentia of this bursa. We seldom find lesions of any kind in which this point is not involved. It seems to be the place where there is the most mechanical stress. It is here that the supraspinatus is at the greatest disadvantage in overcoming inertia in starting the upward motion of the arm. The
sudden contraction of the deltoid may jam this point on the acromion or coraco-acromial ligament if the supraspinatus is not on the qui vive. Here also would come the greatest friction in occupations requiring repeated elevation of the arm. At any rate, lesions of the bursa as a rule are found on the base at this point. I have recorded
none on the roof except a general synovial thickening.
There is a vast difference in the appearance of these synovial villi in life and after death. In life they are often pink or red, but in the cadaver they are limp and colorless and do not readily attract notice. In my opinion their presence is evidence that there has been inflammation and adhesion of the bursal surfaces, followed by resolution of most of the adhesions. They are probably homologues of pleural bands and are remnants of organized exudate. They are very frequently found and are to be expected in the bursas of the type of human being usually found in the dissecting room.
(5) Bands. In a few cases at operation I have found thick, cord-like bands of fibrous consistency similar to the bands one frequently finds in the olecranon or prepatellar bursa. One very typical case was in a man who had for years climbed electric light
poles, usually carrying heavy weights as he did so. A very painful, chronic bursitis with loud friction sounds developed. Excision of the bands restored normal use of the arm. Such cord-like bands are relatively uncommon in this bursa although frequently found in the prepatellar bursa. They must not be confused with the film-like synovial villi spoken of above, nor with the " straps " alluded to under No. 9.
(6) The normal nictitating folds formed by double layers of the movable periphery and described in Chapter I, page 27, may become inflamed and swollen. I have occasionally seen them bright red, resembling inflamed conjunctiva. They are sometimes the sole cause of a mild, chronic, non-adherent bursitis, giving intermittent, elusive symptoms such as twinges in certain motions.
(7) Adhesions. As stated previously, I have come to believe that the bursa, like the peritoneum, possesses the function of rapidly forming protective adhesions to confine inflammation, and also the ability to absorb them and thus restore, in whole or in part, the mobility of the adjacent tissues. For instance, the diaphanous folds which often partially separate the subacromial and subcoracoid portions of the bursa may, when inflammation arises in one portion, wall off the affected part after the manner of water-tight bulkheads in a modern steamer. It is not uncommon to find blotches of calcareous deposit, which have escaped into the bursa, thus localized.
In my experience adhesions never occur in the strictly subacromial portion of the bursa, and are most common in the subdeltoid portion and in the fold partially separating this from the subcoracoid portion. They are seldom very dense in any situation. They are always absorbed or rendered pliable in time by nature's own processes. Frozen shoulders from this cause invariably recover. I have probably relieved the minds of more patients by this assurance than by my best operative efforts on their bodies.
(8) A slight amount of fluid in the bursa may occur in any acute or chronic bursitis, but if on opening the bursa and abducting the arm, a large amount, i.e., several drams spurt out, one may be quite confident that the supraspinatus is ruptured and that there is a free communication between joint and bursa. As in other joints where there is synovitis, we may assume that nature supplies this fluid to reduce friction.
(9) Straps. These are damaged tendon fibers. One sees just over the supraspinatus insertion a circular area about an inch in diameter, which seems to be worn as if from friction. It is ragged and frayed. On close inspection there is a thin strap of fibers running in the same direction as the supraspinatus fibers and really composed of tendon tissue. The strap is perhaps a half inch square, attached above and below to the supraspinatus and lying on it or in it, but separated from it by a space. It is usually separable into a half dozen parallel strands. It can be lifted up except where it is attached at its two ends and perhaps by filmy material on its sides. It is very thin but quite firm. I have not been able to make out positively whether these lesions are caused by friction and consequent inflammation, or are remnants of the effect of the discharge of a calcified deposit in years gone by, or are the results of partial ruptures. If you abduct the arm this little strap will buckle up off the tendon on the top of the greater tuberosity like an inch worm. Section of such a case showed that the deeper parts of the tendon were a series of such "straps" on a smaller scale. The tendon seemed to be split in layers.
Dr. Akerson is studying a series of normal supraspinatus tendons at different ages and has kindly allowed me to have some of his sections. At all ages there appears to be a tendency for the tendon fibers to lie in loosely attached planes or laminations parallel to the joint surface as in Fig. 9. In the pathologic tendon these rifts or separations become complete and "straps" are formed. One receives the impression that normally these bands of tendon may each in turn take the maximum strain as the arm is elevated. Also that any one of them singly may tear or evulse from the denser portion of the attachment.
(10) A deep red, more or less circular zone of turgid membrane lying on the base of the bursa in the region of the supraspinatus facet is a not uncommon finding in the class of cases described on page 216 as tendinitis. Often this zone has a whitish central area which corresponds to the portion of the tendon just proximal to its insertion. The calcified deposits are usually surrounded by similar red, circular zones. Those referred to under this heading differ, because no white deposit is obtained when the whitish area is incised with the point of a knife, nor does any show in the X-ray. In one such case after puncture with the knife a few little rice-like grains of material popped out through the opening. Under the microscope the rice bodies appeared to be bits of necrotic tendon. In another case a little fluid came out under tension. In several other cases I have excised bits of tendon and found invariably the peculiar degenerated condition illustrated in Plate VI.
It will be more appropriate to consider the cause of this condition in the tendon under heading B. The point which I wish to make under this heading is that the red, circular zones are visible from the bursa in both these cases and in the calcareous cases. The deep red, circular zone seen on the base of the bursa is due to congestion of the subsynovial vessels. It is very superficial and does not extend into the tendon, which itself is very anasmic. In fact, the gross appearance of the whitish center in both cases suggests there has been an infarction. The reader should refer in this connection to page 232.
B. CHANGES OCCURRING IN THE MUSCULO-TENDINOUS CUFF ITSELF
.jpg)
(1) Degeneration in the collagen of the tendinous fibers is so common that it is difficult to find in elderly subjects an example of normal tendinous substance. Even in the case which I have used as an illustration of the normal insertion of the supraspinatus (Fig. 9), a few of the fibers showed early changes. Fig. 5, in Plate VI, is taken from this case. It shows small areas of collagen which take a deep red stain with hematoxylin and eosin, and at first sight resemble muscle fibers.
In practically all the bits of tissue which I have taken from the tendons at operation or from the specimens Dr. Akerson has examined, these same changes are found in some degree, whether the specimens came from tissue adjacent to calcareous bodies, partial or complete ruptures, or from the non-calcareous cases which I am disposed to call "tendinitis."
Little pathologic work has been done on lesions of tendons in any part of the body, so there is not much in the literature to help us to interpret our findings. Indeed, there is little to say beyond the fact that hyaline degeneration occurs and is not accompanied by invasion of lymphocytes or leucocytes, or other usual inflammatorysigns. The degenerated areas vary greatly in their staining reactions, which may be as blue as cartilage or as red as muscle with hematoxylin and eosin.
I am convinced that some of the central fibers of a tendon may tear without those which are superficial to it on the bursal side, or beneath it on the joint side, being ruptured. In one case in the living, I opened up a little cavity in the tendon which contained fragments of degenerated or necrosed fibers. There was no apparent opening from the cavity which contained these little bodies, either toward the joint side or the bursal side. They were not calcified. It seems to me highly probable that the calcareous deposits represent nature's failure to heal such internal lesions in the tendon. However, one might take the opposite view that central degeneration first took place; then fragmentation of the degenerated areas; still later calcification of the fragments; finally, discharge into the bursa and, soon after, absorption as described on page 69.
We must at present confess that we do not know what the first step in the retrograde process is. It may be traumatic infarction, or perhaps due to a general toxic condition.
It stands to reason that there must be a stage in the course of the calcified lesions just prior to the time when X-ray evidence can be obtained, when necrotic tendon fibers would be found without any calcium in them. Perhaps some day we shall be able to diagnose such cases, and by simply puncturing the tendon remove the tension and obtain prompt relief. This is certainly possible now as soon as the calcium is dense enough to show in the X-ray. In such cases the little cavity contains only a milk-white fluid.
(2) Calcified deposits. These peculiar and interesting areas are probably the next most common lesions to villi, although in the dissecting room, partial ruptures of the supraspinatus will be found much more often. This is because the deposits are temporary and undergo natural absorption, leaving no evidence behind, unless perhaps defects in the tendons. Many partial and all complete ruptures, on the other hand, leave a permanent defect. In living patients the deposits are probably more common or at least more often diagnosed, because, when pronounced, they show in the X-ray. I am convinced, however, that many are small and escape notice, for I have seen some in very clear films which are not larger than a pin-head and others which cast but a faint shadow, easily missed if they had overlapped the contour of a bone. Many escape notice entirely and perhaps never give symptoms. Some are microscopic. (Plate VI.)
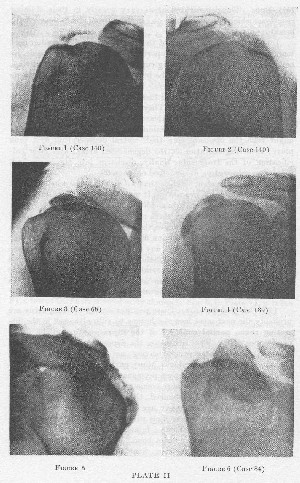
PLATE II. CALCIFIED DEPOSITS
Figure 1. The deposit appears to be double. The larger mass lies in the supra-spinatus tendon, while the smaller mass is in the portion of the infraspinatus tendon which lies, in part, anterior to it. (See Chapter I, Fig. 6.) The long diameter of the latter is probably perpendicular to the plane of the plate. The motions of this arm were free, and without symptoms, although the patient had acute symptoms in the other shoulder, shown in Fig. 2.
Figure 2. The shadow of the deposit consists of a diffuse portion and a small dense portion. The diffuse portion was due to calcined material in the supraspinatus tendon, which had not yet perforated into the bursa, although it was on the point of doing so at the time of operation. It had infiltrated the substance of the tendon and muscle far beneath the acromion. In both shoulders the shadow of the deposit corresponds very well with the normal position of the tendon. The dense portion was probably in the infraspinatus.
Figure 3. Shows a large, dense deposit in a patient with subacute symptoms, who still possessed a normal extent of motion in his shoulder joint, although he had acute pain during elevation when the mass impinged between the tuberosities and the acromion process. The calcified material had not yet escaped into the bursa, although the X-ray shows outlying specks of calcium in the superficial parts of the tendon. As is the case in most instances, the deposit was made up of small, dense masses. The tuberosity shows characteristic atrophy in the trabeculae. At operation in both this case and in that shown in Fig. 2, the floor of the bursa showed a red zone with a white center. Contrast these three figures with Figures 4 and 5, which show the bursa distended with the material.
Figure 4. Should be compared with Fig. 34, for it shows a similar outline of the extruded particles. In some cases, e.g., Fig. 44, the lower portion of the bursa appears to be bilocular, the particles having accumulated by gravity in the fluid at the bottom of these pockets. One should understand that in these figures we detect merely the outline of the bursa, as if in section, but that in reality the bursa lies also in the antero-posterior plane and forms a concavo-convex cap over the tuberosities.
Figure 5. As in the last case, one may be sure that the deposit has burst into the bursa if the bulk of the material shows external to the tuberosity in the unro-tated antero-posterior view.
Figure 6. Illustrates a case alluded to in the text (p. 78) in which a second operation was done. There is a remnant of the deposit still left in the infraspinatus after the first operation, which was on the supraspinatus, but the long, oval deposit is in the subscapularis and was removed at the second operation. Compare this figure with another case where the deposit was in the subscapularis and is shown in the outline drawing, Fig. 43.
The deposits do not arise in the bursa itself, but in the tendons beneath it. Most instances occur in the supraspinatus tendon close to its insertion, but a considerable number are found in the tendon of the subscapularis and in the tendons of the infraspinatus and of the teres minor. I formerly did not identify them in these tendons. As will be seen later, one does not see these tendons in operating, and at first I contented myself with removing the deposit and making no particular effort to determine its exact situation. It took me some years to realize how easy it is to determine the situations of the tendons when operating by placing the arm in exactly the mid-position between external and internal rotation and palpating the bicipital groove. Since, after the bursa is opened, one usually has no difficulty in locating the deposit by the circle of blood-red congestion about its whitish or yellow center, it has seemed superfluous to ascertain which tendon contained it. I later learned that there might be two or more deposits each in a different tendon. In one patient failure to remove both at the first operation resulted in a second attack of acute symptoms and a second operation. On page 230 the importance of accurate X-ray localization is emphasized.
The size of the deposit varies greatly, ranging from that of a pinhead to a shadow, two or three inches long, of the supraspinatus tendon and muscle as in Plate II. Such large shadows are very rare, and the deposit is seldom bigger than a lima bean. The consistency varies also and may be that of a milk-white fluid or of a hard, yellowish crystalline substance. Usually it closely resembles in color and consistency ordinary zinc ointment. Sometimes it is cheesy and yellowish, like the contents of a wen. In acute cases- it is not difficult to remove, but in some chronic cases of long standing it is very gritty and seems incorporated in the fibers of the tendon so that one cannot curette it all out without removing much semi-normal tendon with it. One sees whitish, stringy fibers in the little pit from which it is being removed. Sometimes it shells out very easily with a definite contour. In my own operations I have avoided removing any tendon, preferring to leave some of the deposit in the fibers, than to excise tendon which might return to normal and become of use in future function. Brickner has removed enough for sections, and Moschcowitz has studied them. Harbin has not hesitated to remove some tendon and reports good results in spite of this. On a few occasions I have found the deposit surrounded by a small amount of granulation-like tissue, largely composed of foreign-body giant cells, but in these eases the deposit had probably perforated into the bursa.
Several times I have had careful chemical analyses made.
Dr. James L. Stoddard made for me an analysis of the material from one of these cases.
"The following report on the bursal deposit shows it to be a mixture of calcium phosphate, calcium oxalate, and organic matter, mostly fibrin.
Gross: A pasty, white mass, in part blood tinged, springy and a little elastic on stretching, moist, with an extremely fine, even texture, and with no evident structural elements which hinder division at any point.
Microscopic: Small ovoid colorless bodies, varying enormously in size. Some are at the limit of vision with an oil immersion lens, and show marked Brownian motion; all gradations exist up to bodies several times the diameter of a red cell. They are all the same in qualitative appearance. They are slightly refractive, less so than fat, have usually a somewhat irregular oval shape, but the edge is always smooth and even. Nothing but the bodies is visible in the specimen.
Chemical—Qualitative: No color with Sudan 3; hence not fat.
Insoluble in acetic acid, alcohol or ether.
Soluble for the most part in fairly strong HC1.
On heating to yellow heat, chars, smokes, and burns briefly with a yellow flame, and gives a burnt feather odor. Leaves a gray ash.
Ash dissolves easily in weak acetic acid with evolution of C02, showing original substance to have contained oxalate.
Gives no murexide test for uric acid. No test for cholesterol (Lieberman-Burchard test).
Solution in strong KOH acidified with acetic acid gives off slight trace of H2S, detected on lead acetate paper. This is probably due to presence of fibrin, which also explains the consistency of the deposit.
Solution of ash gives heavy phosphate test with ammonium molybdate.
Chemical—Quantitative: A small sample of the deposit was ashed, weighed (weight 86 mg.), dissolved in HC1, filtered from char, ammonium oxalate added, the solution neutralized, and the precipitate analyzed quantitatively for calcium as in the blood calcium method (Clark's modification of the Kramer-Tisdall method).
The filtrate was made acid with acetic acid, and a calcium acetate solution added to precipitate the excess oxalate which would interfere with the phosphate determination. The filtrate from this precipitation was analyzed for phosphate by the blood phosphate method (Brigg's modification of the Bell-Doisy method).
"Result: Calculated back to Ca3(P04)2 and Ca204, H20 gives respectively: calcium phosphate 55.8%, and calcium oxalate 44.2% of the inorganic matter of the dried, unashed specimen. The amount of organic matter was not determined. Of the ash there was 14% not to be accounted for by figuring all the phosphate as calcium phosphate, and the remaining calcium as carbonate. Part or all of this 14% was due to char, and part may have been due to other inorganic matter (perhaps some magnesium salts, etc.). (The ashing was done at the lowest possible heat, but of course some of the calcium carbonate may have decomposed into oxide, which would raise a little the undetermined fraction.) One of the most interesting features is the peculiar microscopic appearance of the specimen, with this non-crystalline precipitate of fairly definite shape."
Maxwell Harbin (Arch, of Surg., Vol. 18, No. 4, P. 1491, Apr., 1929) reports a case which from the X-ray film is very clearly a case of perforation of one of these deposits into the bursa. He made a rather extensive excision and gives the following report of the chemical analysis of the specimen, together with a low power photomicrograph.
"The bursa, as well as the necrosed tendon (Fig. 8), was excised. It is of interest to note the considerable variety of earthy substances which exist in the necrosed tendon. Inorganic phosphates were present to a considerable degree. Calcium was easily discernible with a trace of calcium, iron, carbonates and chlorides. The specimen was composed of tough, white fibrous substance covered in certain areas by a cream-colored cheesy substance. A few grit-like particles were found in the cheesy material. Some hardened blood was present. Analysis of tissue removed from the supraspinatus tendon showed the following:

"The white fibrous substance was apparently dense fibrous connective tissue. The yellow cheesy substance was composed of fat, protein and a fair amount of calcium phosphate." Comment by E. A. C.: Confessedly Dr. Harbin had excised some tendon and fat, and the analysis was not made from the pure deposit as in my case.
One of my assistants, Dr. T. W. Stevenson, made the following observations:
Study of a Calcareous Deposit
A little of the material was suspended in normal saline and observed under the microscope. Many small bodies of variable size, mostly round or oval in shape, were seen. The smallest were the size of bacteria or smaller and the larger ones were about the size of white blood cells. Scattered over the slide were many large, round or oval bodies 10-15 times the size of a white cell. They presented a peculiar appearance in that they were concentrically striated. The appearance resembled that of the gall stones pictured in MacCallum's Pathology. The center of these bodies is slightly clearer than the periphery. This central nucleus (?) resembles a white cell and is about that size. The concentric rings are very distinct, but two or three in each body are more pronounced than the others.
When a little of the material was suspended in concentrated sodium hydroxide solution, the bodies were turned slightly more yellowish. The striations were more marked. No dissolution or other change occurred up to one hour.
Concentrated nitric acid caused no change.
Glacial acetic acid caused no change.
Thin smears were made and fixed by heat. They were stained and the following results noted:
Gram's Stain: No organisms were seen. The calcareous bodies decolorized and were stained an even red with no striations visible.
Methylene blue stained the bodies an even blue and concealed the striations.
Ziehl-Neilson stain showed no acid fast organisms or bodies.
Stern of Cleveland has reported that these deposits are modified fat, but I can find no evidence to support his contentions.
Dr. Robert Chambers was kind enough to investigate some of the small bodies for me with his dissecting microscope. He found, when he attempted to pull them apart, that they were quite elastic and sprang back to their original shape.
I have repeatedly made microscopic examinations of fresh specimens of the material removed and they always consist chiefly of the little, round and ovoid bodies above described. I have never succeeded in dissolving them in ether. Their real character remains a mystery to me, but I am satisfied they are not fat.
Moschcowitz in 1915 said: "The calcification is present either in the form of discrete, sharply circumscribed, sand-like masses, embedded as it were in a cavity within the tendon; or as diffuse, finely granular masses, shading imperceptibly into the surrounding tissue structure; or as finely granular amorphous material, lying within the tendon or the granulation tissue." Concerning another case he said: "In no specimen was the slightest tissue reaction noted, in the form of round cell infiltration, granulation tissue or the formation of new blood vessels."
It seems to me that the latter statement is more characteristic of the early uninflamed stages in the tendon when the trouble is forming and the bursa is not yet involved. The first description is that of a more acute case when the deposit has caused a reaction in the base of the bursa. It seems to me probable that new blood vessels, etc., proceed into the tendon from the synovia. In such cases, unless the bursa is involved, it is striking that blood vessels, lymphocytes and the usual microscopic phenomena of inflammation are lacking, and yet there is clear evidence of degenerative change. I hazard the suggestion that it may be found that tendon repair differs from the repair of other tissues in this respect; i.e., that necrosis must first proceed to a point where it involves an adjacent vascular tissue before vascularization will take place.
Moschcowitz did not definitely state his opinion on the question of precedence of lesion or trauma, for he was evidently influenced by Brickner's belief that this calcification process was a prompt reaction to a trauma. My own belief is that the deposit has probably been present long before the trauma with which it is associated by the patient.
Moschcowitz continues: "The necrotic tissue can have only two sources: (1) Degeneration of the blood and serum consequent upon the primary trauma. (2) The breaking down by coagulation necrosis of the tendinous structures." He excludes the first because there is no blood pigment; the tissue is too homogeneous and plastic in appearance; the line of continuity of the necrosed portions with the solid portions is a gradual one. He also states that it used to be generally accepted that calcification never occurs in any but dead or inert tissue, but that in consequence of recent experiments, which he quotes, it seems that calcification may be a matter of only a few days in areas rendered anaemic by tying arteries. Yet he says it does not follow experimental suture of tendons.
It seems to me that we are indebted to Moschcowitz for the best statement of the pathologic findings, but that he has been too strongly influenced by Brickner's clinical belief that in these cases calcification is an immediate result of trauma. He also quotes me as believing this, but I do not recall that I ever did believe it, and I certainly did not state this in my writings. I did believe, and do still, that some slight injury, long before, may have pulled the fibers apart and started the process. Since tendons contain few blood vessels, evidence of hemorrhage is not required to support the likelihood of this theory.
There are two other interesting points in Moschcowitz' paper. One is that he was unable to find in the literature of pathology that any effort had been made to study the minute pathology of these lesions. He was only able to find Wright's report (on one of my cases, and which I had quoted) and another by Wrede, which was inconclusive. The second is that he prophesies that since in other tissues where one finds calcification one eventually finds some ossification, we should presently find ossification in an instance of this lesion. I have not yet been able to find such an instance proved microscopically. One must not be deceived by bits of the tuberosity in a retracted supraspinatus tendon.
Similar formations are sometimes found in other tendons, as in the quadriceps and the gluteus medius, and I know of one case in the flexor carpi ulnaris. Dr. .J. H. Wright told me that a similar pathologic process was found in the heart valves.
The question of whether infection has anything to do with the condition has ceased to interest me, as I have always closed the wounds and have never seen even mild sepsis develop. Many times I took cultures which were always negative. Nor have I been able to definitely associate the condition with distant foci as evidence of toxaemia. Of course, many patients have bad teeth, but in no instance has there seemed to be any association, for as soon as the deposits are removed the patients promptly recover, whether the teeth have been extracted or not. In one instance extraction of a tooth was at once followed by acute symptoms in the shoulder, which soon subsided and disappeared altogether. However, I strongly recommend every patient with bad teeth to have them attended to, although I do not consider the causative connection scientifically established.
There is no constitutional condition which I have associated with the lesions, for they occur in the lean or the fat, in the active or sedentary. My chief reason for believing that they are primarily due to trauma or overuse is that their pathology may best be accounted for on this hypothesis. Furthermore, I do associate them to some extent with occupation, for they occur in people who habitually use their arms in semi-abduction, as stenographers, accountants, machine operators and surgeons. I think that automobile driving may have a tendency to encourage this formation. In fact, any occupation or avocation which requires undue use of the abducted or elevated arm.
(3) Defects due to ruptured supraspinous tendons. In spite of my known interest in the subject and the goodwill of many friends in active surgical practice, I have never seen, either on the operating or autopsy table, a fresh rupture of the supraspinatus tendon. It merely happens that no one recognizes these cases in time. I have seldom operated within three weeks after the injury, although I strongly believe in immediate operation. The earliest case was three days after the injury, and in this case, unfortunately, there had also been a prior one. Decided changes occur in the first few weeks, so that one finds the ends of the torn surfaces covered with fresh tissue which disguises the exact anatomic relations of the parts. However, experience in operating at varying intervals after the trauma, combined with dissections on the cadaver, has given me a fair idea of the method of healing which nature attempts. We must examine again the normal anatomy.
The continuity of the semi-circular conjoined insertion of the four muscles (see p. 17) is interrupted by the groove for the biceps tendon which separates the two tuberosities and theoretically the insertions of the subscapularis and supraspinatus. The facets of insertion of these two muscles are widely separated in anatomic diagrams, but as a matter of fact, their common expansion bridges the groove and makes them continuous, although thin just over the groove. Ruptures almost always involve this portion over the groove and it is very often the internal limit of the rupture, which as a rule extends from this point outward, involving the portions of the cuff made up of the supraspinatus and part of the infraspinatus expansions. Occasionally the tear crosses the bicipital groove and involves the subscapularis portion of the conjoined tendon. In at least one dissecting room specimen the tear extended inward from the groove and involved the subscapularis portion alone.
When one opens the bursa in these cases the biceps tendon may or may not be exposed, according to whether or not the tear extends across above the bicipital groove. It is usually to be found just under the edge of the inner side of the rent. If it is exposed it is seen as a bright pink band crossing the bluish surface of the shining articular cartilage. It is not only pink and inflamed looking, but may be twice its natural size. One finds that below and above the point where the biceps tendon is exposed by the retraction of the ruptured supra-spinatus, it is still of normal size and white and shiny. When not exposed, but lying just under the edge of the portion not ruptured, it is not abnormal looking. Frequently it cannot be found, for it has been torn off its attachment on the glenoid and has been pulled by its own muscle belly down into the bicipital groove. The proximal end sometimes sticks in the upper portion of the groove, and at other times retracts way down it and curls up in a coil just above the muscle belly. Occasionally it is found to be much frayed, which probably indicates repeated jamming between the head of the humerus and the acromion. Sometimes the frayed edges are adherent in the groove, and have little rice-like bodies attached to them.
From what I have said about the cuff of conjoined tendon in which the tendons of each muscle and the capsule are welded intimately, and since ruptures always occur in this portion, it will be more readily understood that when I speak of any one tendon as rupturing I mean the portion of the cuff represented by that tendon. Since the gap of the rupture is held on each of its edges by the conjoined tendon, the retraction of the muscle makes the rent triangular. The interweaving expansions of the tendon on each side still hold it to a certain extent, and the pull of the muscle is distributed on the conjoined tendon on each side as if it had a Y attachment. The middle of the inverted Y retracts farthest and the sides slope toward the base on the tuberosity. The shape of the whole rent is therefore roughly an equilateral triangle, with its base on the tuberosity and its apex disappearing under the acromion. The width of the tear is the width of the base; restoration would be made if the apex were sutured to the middle of the base. The base itself is inflexible, being either the bony seat on the tuberosity from which the tendon was evulsed or an inelastic stub of tendon still attached to the tuberosity. The size of this triangular rent varies from a half inch to an inch and a half base. Sometimes only a few fibers are torn, and at other times most of the conjoined tendon. In one case I found that the whole cuff with all the tendons had been evulsed, and that the head of the humerus was free under the deltoid. (See case report on pp. 389, 390, 391.)
A skin wound of triangular shape healing by second intention, i.e., granulation and epithelialization from the edges, becomes rounded before it heals; so do these triangular defects in the supra-spinatus, so far as the edge of the rent is concerned. They differ from the skin defect because there is no bottom or bed of granulations, so must heal entirely from the periphery, and complete closure of the hole is therefore unlikely. In the skin ulcer this peripheral healing is epithelial and spreads over the surface of the granulations on the base as ice, beginning at the edges, skims over a pond. In the tendon defect the peripheral tissue is fibroblastic not epithelial, and fibroblastic reconstruction is dependent on a new formation of blood vessels instead of mere multiplication of cells to skim over another tissue which will feed them. Now it happens that tendon is a tissue in which there are exceedingly few blood vessels to form the basis of new granulations, so that the conditions for healing are still more unfavorable. I have already stated that it is my own belief that tendon repair does not usually take place from within, but from the synovial or areolar tissues adjacent to it. It is likely, therefore, that the synovial covering acts in these cases something like epithelium to cover the edges, and also as an agent to expedite the new supply of blood vessels. At any rate, I have had the opportunity to see on the operating table the appearance of these rents at various stages from a few days to two years after the accident. Even three weeks after the rupture, the triangular appearance is sometimes a little rounded by bridging of the corners and extension from the sides of an almost transparent new tissue, presenting a falciform edge toward the center. In later cases this edge is harder and more extensive, but always presents the falciform margin, which lies on the cartilaginous joint surface in the manner of the semilunar cartilages of the knee joint—clearly to avoid friction.
Obviously, as this circle gets smaller, either by the contraction of the tissue of which it is composed (cf. contraction of surface scars), or by more tissue forming toward the center, the smaller and more circular the defect becomes, until possibly the hole between the bursa and the joint might be entirely closed. Assuming that there is still a stub of tendon attached to the tuberosity, it seems possible that healing in this manner would eventually occur in young, well-vitalized tissues, but in the aged, with barely vitalized tendons, little change would tike place after the first few weeks. This supposition is strengthened by reference to the age table, which shows that I have never operated on a young man and demonstrated a rupture of the tendon.
In those cases in which the tendon is actually evulsed from the facet, a complete circle with a falciform edge is not formed as healing progresses, for the bone forms a defect in the circle. The base of the former triangle is the bone of the tuberosity. It may be bare and as a rule has no granulations; sometimes there is a little velvety tissue on it. On microscopic section of the bare facet, one finds a little skim of fibrous tissue over the spongiosa, and that is all. As a rule there is a little plaque of dense bone beneath this, and at the periphery of the defect some raised "productive" bone. These bony changes are shown in the X-ray. Healing in these cases would appear to be at still more of a disadvantage than when a stub of tendon is left on the tuberosity. It is not unusual to find both, some stub and some bony defect. From the operator's point of view a stub of tendon is a great advantage, for where evulsion has occurred he must drill the tuberosity in order to suture the tendon. A knowledge that a falciform edge is present is also important for the operator, for in most cases he must remove it and pare down to the real tendon tissue before he sutures. The new tissue in this falciform edge is seldom strong enough to hold a suture, and would be in the way of the sound tissue. (Fig. 12.)
Referring to Fig. 6 will help the reader to understand the points at which rupture or evulsion is likely to take place. The figure shows that the insertion of the tendon into the bone is very superficial, and the shell of the surface of the bone is very thin. Under high magnification very many minute prolongations of the tendon are inserted into this thin shell of bone. (The structure suggests to my mind a room full of people hanging to the ceiling by having all their fingers deeply thrust into the plaster as into finger holes in a bowling ball.) As a practical matter this network of attachment to the tuberosity does hold against excessive pull except in elderly people when the attachment is pulled out. In most of the cases I have seen at operation it was apparently evulsed at the line of junction, but soon after the injury a stub of tendon would probably have been found. Such stubs probably slowly disappear.
Referring again to Fig. 9, it will be seen that stress on the supra-spinatus tendon in the direction of its normal pull may result in four different forms of break in continuity:
a. The tuberosity, facet and all may be pulled away. This may occur without making a communication between the base of the bursa and the joint. Since the fixed portion of the base of the bursa is on both tuberosity and tendon, it is likely that the whole bursa follows the displaced tuberosity, and the bony gap is filled in by callus from the peripheral torn periosteum. (See p. 317.) I am quite sure that this is the rule, although my opinion is formed on that very untrustworthy guide, "clinical experience." Cases of fracture of the tuberosity get well much more promptly and with less pain than do ruptures of the tendon, and differ in their minor symptoms from the latter. Moreover, in the two cases cited I have opened the bursa and felt beneath its unruptured base the fragment of tuberosity. In most fracture cases the bursa is not involved because it is higher than the usual line of fracture. (See p. 273.) It seems to me probable that in all cases where the tuberosity is involved, whether it is broken off alone or with several fragments, that the line of cleavage in the bone is just external to the firmly attached base of the bursa, which in fact strengthens the bone locally like a patch. In other words, I think that if one opened the bursa by my routine incision in a series of fresh cases of fracture of the tuberosity, he would not find the bursa full of blood and communicating directly with the two raw fractured surfaces and thus into the joint. Sometimes this would be true when the fragment as shown by the X-ray is drawn inward as far as in Fig. 35, but not in the usual case as in Plate IX.
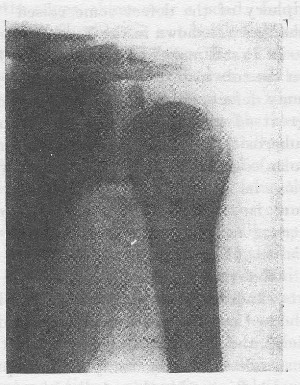
FIGURE 35. RETRACTED FACET AND DROPPING SHOULDER I have found this Rontgenogram, unlabeled among my papers, so that I cannot give, as I usually have in my other illustrations, a statement that the condition was proved by operation. However, the picture is so characteristic of a retracted supraspinatus facet that I do not hesitate to use it. Such a condition is far more serious than most of the major fractures (Fig. 59). Even without knowing the history in such a case I should be confident in saying, from the X-ray alone, that the patient has a post-dislocation condition, where there is "dropping shoulder" due to deltoid paralysis and where the supraspinatus facet of insertion lias been pulled by the muscle beneath the acromion. It also shows some bone formation from shreds of periosteum retracted to a lesser degree by the adjacent tendons. As in cases 71 and 115, the dislocation has probably not been really reduced. These appearances indicate operation.
b. Evulsion may occur at the point of insertion and the superficial part of the facet be carried inward by the retracted tendon. Since this little shell of bone would show very faintly in the X-ray, and also since it would have been absorbed in the long-standing cases which form the bulk of my experience, I cannot speak very positively about it. In a few cases I have seen remnants of it attached to the retracted end of the tendon, and I have often noted its absence on the tuberosity. In some cases it seems that the minute, finger-like processes are evulsed from the bone without taking the bone with them. Occasionally part of the tendon is evulsed, leaving bare bone, while the remaining portion leaves a small stub on the tuberosity.
c. True rupture of the tendon leaving a stub on the tuberosity usually occurs at the narrowest place shown in Fig. 6, leaving the broad, semi-cartilaginous fibro-cartilage still attached to the bone as' a stub. This amount is barely sufficient to permit a good hold with a stitch. I have occasionally seen a larger stub, perhaps three-quarters of an inch in length. In these few cases this larger stub was very vascular and of deep purplish red color like a cock's comb. On one occasion such a stub popped out of the wound as soon as the roof of the bursa was incised. The vascularity of such a stub sug
gests that there must be a considerable blood supply in the bony facet. The desiccated bone shows many vascular channels in the sulcus, and near the upper end of the bicipital groove. Both those cases in which there is evulsion and those in which a stub is left necessarily have a direct communication established between the joint and the bursa. In cases where bursa and joint communicate there is always more or less straw-colored fluid in the joint which washes back and forth into the bursa, rising in the bursa when an effort is made to raise the arm, and falling back into the joint as the arm is relaxed and lowered. This process dilates the bursa and in extreme cases leads to hygroma of the shoulder, as described on p. 478.
d. A fourth condition of great clinical importance consists of those cases in which a portion of the tendon is torn to a degree insufficient to tear the base of the bursa itself, so that a film of tissue is left between the joint and the bursa. I allude to these cases as "partial" ruptures or "rim rents." Repair takes place to a certain degree from the thickening of the film of bursal base. I have found few such cases in the living, probably because they do not cause a degree of disability to make me advise operation, but I have frequently seen this condition at autopsy. If one removes the head of the humerus with the short rotators attached and examines the sulcus which surrounds the articular edge, one finds the attachment of the supraspinatus extremely thin, so that when held up to a bright light the attachment is found to be Y-shaped and the central portion between the limbs of the Y is diaphanous. The sulcus at this point is correspondingly broad instead of being a cleft, as it is in the normal joint (Fig. 10). It appears that the portion of the tendon on the joint side, together with its joint synovial lining, has pulled off, leaving the bone bare.
I believe this fourth division accounts for many of the industrial shoulder injuries which recover after a few weeks or months, and which I have in the past classified as relatively trivial cases of traumatic subacromial bursitis (see Plates III and IV, pp. 101 and 102).
It seems legitimate to assume that in such injuries as almost or quite cause a dislocation of the shoulder, the synovial reflexion and the portion of the tendon on which it is reflected, might be torn away from the articular edge, leaving the bone trabecule bare at this point. There would be slight bleeding, which might gradually fill the joint and distend it. This hemorrhage would in turn be replaced by an excess of synovial effusion, which might be kept up by the individual continuing to use the arm. Motion might prevent the formation of fibrin to act as a basis for new granulations and fibrosis in the bed of bone. Even if pain were sufficient to start scapulohumeral spasm, the effusion might hold the parts apart and prevent proper healing. If the patient were old, and the tissues already weak, healing would be even more unlikely. At any rate, it is very common to find at autopsy that the sulcus is bare.
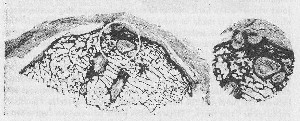
FIGURE 86. VOLCANOES AND CAVERNS
Deeper section through the same tuberosity as that shown in Plate V, Figure 1. The ends of the canals of invasion of vascular tissue appear as caverns. As these caverns and volcanoes are frequently found in X-ray films in cases of tendinitis, as well as in cases primarily due to rupture of the tendons, intensive study should be given to them.
C. CHANGES IN THE GREATER TUBEROSITY
.jpg)
(1) Excrescences. Pathologic changes in the tuberosity may readily be detected by the X-ray. In many cases of old, complete ruptures of the supraspinatus and in some cases of partial rupture, the relative thickness of the tendon and of the tuberosity is changed, so that there is a notch in the base of the bursa. Thus the tuberosity forms a distinct eminence and may cause a jog and friction as it passes upward under the acromion. The result is a stimulation of the bone cells in the tuberosity and irregular excrescences form at the region where undue friction occurs. This new formed bone is very spongy and probably later atrophies, because in the very old cases one finds that complete recession of the whole tuberosity has taken place. Atrophy of the tendon without actual rupture might cause enough irregularity in the base of the bursa to begin a little irritation. A vicious circle of atrophy of tendon, inflammation of tuberosity, osteitis, excrescences, greater jog and greater friction, greater atrophy, etc., might be established. At the same time hypertrophic changes on the acromial edge are stimulated.
(2) Caverns. Very frequently where this superficial osteitis occurs on the tuberosity, there is also absorption of the bone beneath its surface. This absorption of the bone results in the formation of little caverns which contain vascular tissue. I am inclined to think that they represent the early stages of what I call recession.
(3) Eburnation. By eburnation I mean an increased deposit of lime salts which result in the hardening of a definite area of the bone. Such areas of eburnation are frequently found at the insertions of these tendons in working men. In the X-ray a heavy plaque of bone is shown where the tendon is inserted in the sulcus. In some cases where the fibers of insertion have been damaged, there appears to be an increase of this bony deposit, so that when this is found in a case of suspected rupture, it is a confirmatory sign. It is not, however, of much importance practically. In my opinion, this appearance is evidence of the existence of low-grade, chronic inflammation, and I think that it is possible that the increase of this bony substance may interfere with the nutrition of the finger-like processes which hold the tendon in the bone at this point and tend to weaken the hold which these processes have there.
(4) Bursal osteitis. Osteitis caused by this irritation on the tuberosity may sometimes involve the outer side of the tuberosity as well as its tip. The base of the bursa may be the seat of chronic inflammation, so that irregularities will be shown by X-ray on the appropriate portion of the tuberosity, external and below the insertion of the tendon, on the outer aspect of the bone.
(5) Recession. I have referred above to the atrophic changes which take place in the sulcus and tuberosity long after ruptures of these tendons have occurred. It is highly probable that most ruptures occur at the line of junction of the tendon tissue with the palisade-like fibrocartilage adjacent to the bone shown in Fig. 9. When I have operated within a few weeks after the accident, this stub of tendon was usually present. In the very late cases, however, the tuberosity has usually been found to be quite bare, and not only bare, but atrophic. Instead of showing a normal sulcus and tuberosity, these structures are more or less leveled off, or, as I prefer to say, there has been a gradual recession of the tuberosity after the stub of tendon has worn away or been absorbed. The sulcus and tuberosity were no longer of use, but were actually an impediment to elevation of the arm. Without the pull of the tendon to fulfill its normal functional demand, the tuberosity had gradually disappeared. In the very old cases, such as many of those Dr. Akerson found at autops}', or the case mentioned on page 108, the recession of the tuberosity was so marked that one could hardly tell, by superficial examination, where the old cartilaginous edge ended, or where the area normally occupied by the sulcus and tuberosity had been. This region now wa.s smooth, covered with a thin fibrous layer, and continued the rounded contour of the articular head. This recession of the tuberosity may be detected also by the X-ray. Note the dotted line in Diagram C and also Plate IV.
(6) Trabecular atrophy. In all long-standing lesions of the bursa, whether or not they are due to rupture of the tendons, the X-ray shows that the trabeculae beneath the base of the bursa are more or less atrophied. This produces a dark area in the X-ray film which corresponds with the portion of the tuberosity on which the base of the bursa rests. In the normal bone the trabeculae are, to be sure, less dense in this region than in other parts, but where the atrophy is pathologic, the outline of this more translucent area is indefinite and not as plainly marked as in the healthy bone. I presume that the trabecular are absorbed because there is chronic congestion of the small vessels of the marrow spaces in the region. This kind of atrophy is sometimes very marked in acute cases of bursitis due to calcified deposits. In such cases it slowly disappears after the lesions have healed.
.jpg)
D. CHANGES WITHIN THE JOINT ITSELF
(1) The common lesions of the long tendon of the biceps have been alluded to on p. 85.
(2) Rupture on the joint side of the tendons (rim rents). We have already considered under B, lesions of the tendons at this point, but since they do occur here, they necessarily involve the joint. Normally the true joint cartilage forms a very sharp angle with the insertions of the tendons, as shown in Fig. 10. Fig. 9 shows some of the fibers beginning to tear at this synovial reflection. Diagram D shows an extensive tear so that the rent-has come through to the most superfici fibers of the tendon. The reader should visualize this vertical section so as to understand that the rent also extends along the curve of the edge of the joint cartilage to a considerable extent, leaving the sulcus bare, perhaps for an inch or more. This condition I like to call a "rim rent," and I am confident that these rim rents account for the great majority of sore shoulders. It is my unproved opinion that many of these lesions never heal, although the symptoms caused by them usually disappear after a few months. Otherwise, how could we account for their frequent presence at autopsy?
(3) Eburnation of the sulcus has already been spoken of under the last heading, but it is unavoidably listed here again because it lies at the periphery of the joint.
(4) Raised articular edge. Not infrequently we find in elderly subjects, a very slight, rounded, corona-like elevation of the edge of bone under the articular cartilage. It is difficult to say whether it is really pathologic in character. It might be regarded as evidence of a chronic arthritis. However, it is frequently present as shown by X-ray, in joints of which the patient makes no complaint. So far I have been unable to attribute any clinical significance to it.
(5) Adhesions of the extensions of the joint. The reader will recall the so-called bursal extensions of the joint which lie beneath the infraspinatus and subscapularis. It is highly probable that the margins of these, especially the margins of the one beneath the subscapularis, may be stretched or torn so that habitual dislocation may readily occur. On the other hand, adhesions between their surfaces would necessarily limit the motions of the joint. I mention these extensions because some future investigator may be able to make some observations of clinical importance concerning them, but my personal experience with them is nil, for I have not even studied the question systematically on the cadaver. Albert (1893) mentions a case of tumor in the axilla caused by distention of the subscapularis bursa, but I have never observed such a case.
(6) Fluid in the shoulder joint is considered on page 115. The chief point which I wish to make in regard to it at present is, that in elevation of the arm the lower portion of the capsule is stretched tight and fluid is forced upward into the rim rents or, if there is a communication through the whole tendon, into the bursa itself. Theoretically, if there is fluid in the joint and the tendon is not ruptured, elevation of the arm should also tend to dilate the bursae beneath the subscapularis and infraspinatus.
.jpg)
E. WHEN THE MUSCULO-TENDINOUS CUFF HAS BEEN RUPTURED
So THAT A FREE COMMUNICATION HAS BEEN ESTABLISHED
BETWEEN THE JOINT AND THE SUBACROMIAL BURSA
The considerations under this heading are merely presented as a review of the others, with the particular idea of accentuating what I believe is nature's method of compensating for these lesions, i.e., dilatation of the bursa by joint fluid, gradual absorption of the tuberosity and atrophy of the stub of tendon in order to form a new, smooth surface.
(1) Indicates the fibro-synovial edge which is formed very soon after the injury and which must be pared away before the tendon is sutured.
(2) Erosion of articular cartilage. It is obvious from what has been said that after rupture of the musculo-tendinous cuff, more or less articular cartilage will be exposed on the base of the bursa, and that the cartilage at this point would be subject to contact with the acromion when the arm is elevated. In old cases at operation or in specimens of extensive tears found at autopsy, one frequently sees a superficial erosion of the joint cartilage with clearly marked outlines separating it from the undamaged surface. These areas of erosion are consistently limited by the size of the rent. Perhaps it is better to say that these areas of erosion are always somewhat larger than the rent, because in different degrees of rotation of the humerus different parts of the articular surface can be exposed through the same rent to pressure on the acromion as the arm is elevated. In practically all the cases where an extensive rupture exists, there is some osteitis on the edge of the acromion, which would increase the wear and tear made by the articular surface touching the acromion through the gap. This erosion of the joint surface is always superficial. It is possible that in some cases the process is reversed. It may be that the rough acromial edges wear through the tendon.
(3) Is the stub of tendon which remains on the tuberosity for some weeks or months after the injury, but since it is functionless, eventually disappears.
(4) Represents the dotted line which limits the recession of the tuberosity.
(5) Is the fluid in the dependent axillary portion of the capsule.
In the above description of the pathologic changes which I have observed in this region, I have endeavored to confine my remarks to the essential features which I am sure that any one who is earnestly studying these joints will be able to verify. Such a student may also find many other atypical little irregularities in the tissues close to the lesion in the tendon, which I have not thought it worth while to describe. However, when one has examined a considerable number of joints, these changes will seem relatively unimportant and entirely secondary to the lesions described above. One must not allow one's self to be deceived by these secondary changes, although sometimes the congested, inflamed synovial folds are the most striking lesions visible.
Before closing this chapter it is well to add a word about the question previously brought up as to whether some form of necrosis in the tendons themselves, such as age induces in the walls of arteries, is largely responsible for the various lesions or at least for their failure to repair. The facts that most of my cases are aged, many are bilateral, and that I have observed no cases in young people are strongly suggestive of this idea. Moreover, the traumatic cases as well as the calcified cases show a similar degeneration of the tendons under the microscope, although many of the latter are in somewhat younger people.
It seems possible that these lesions may occur merely from gradual deterioration of the musculo-tendinous cuff. The frequency with which they are found at autopsy would suggest this, as well as the reasons spoken of in the last paragraph. When a tendon has disintegrated to a great degree of weakness, even a slight effort might break away the rest of it. However, this is not usually the case, for all but two of my operated cases of complete rupture of the supraspinatus gave a very clear history of serious trauma. Dr. Wilson's cases also had histories of trauma, with one exception. The findings at operation in the three exceptions were similar to those in definitely traumatic cases. Moreover, the results obtained by operation were excellent; in fact, both my cases were demonstrated at a medical meeting as perfect results. How can we account for this combination of a non-traumatic history with typical operative findings and excellent results? If the lesions were caused by a progressive disease we should not expect good results.
It happens that in both of my cases I strongly suspect that the injury had occurred when the patients were drunk. Since I believe that the usual cause of this injury is a sudden attempt at elevation of the arm to maintain balance during a fall, I think it is quite likely that such an injury may occur to a reeling drunkard. Therefore, I feel that before we say that these lesions are ever non-traumatic, careful inquiry should be made into the possible chance that the injury occurred while the patient was intoxicated. The early symptoms are not necessarily very marked, and would readily be masked in a case of a steady drinker.
Goldthwait has suggested that faulty posture underlies the weakness of the tendons. I am convinced that overuse of the arms in abduction without giving the tendons time to let their circulation do its duty, because they are perpetually stretched, has much to do with these lesions. I have no doubt that trauma may rupture a healthy tendon, but I think rupture from trauma occurs in the great maj ority of cases in aged tendons made weak by overuse, age, or toxic conditions. Dr. Akerson suggests that long-continued disuse might weaken aged tendons to such an extent that they would break under very slight strains and perhaps without much pain.
Whether or not injury precedes or follows degeneration in the tendons, it is a fact that complete rupture of the supraspinatus tendon may be diagnosed and even in late cases may sometimes be successfully repaired by surgery.
PATHOLOGIC HISTOLOGY
In studying the lesions that have been discussed, we should first have some idea of the normal microscopic landmarks which may become altered by injury or disease. The diagram (Fig. 37) should be compared with Fig. 9 in Chapter I, which shows an enlargement of the normal insertion of the supraspinatus tendon in the region where pathologic changes usually take place.
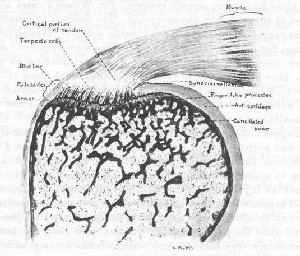
FIGURE 37. DIAGRAM OF MICROSCOPIC REGIONAL LANDMARKS
The relative sizes of the structures and cells have been altered in order to simplify the figure, which should be compared with a photograph of an actual section of this region (Fig. 9).
1. "The Critical Portion" of the tendon is the half inch proximal to the palisades. It is in this region that calcified deposits gather and where complete rupture frequently occurs, although partial ruptures usually begin at the edge of the cartilage. As has been said, even under the microscope one cannot distinguish, in this part of the tendon, between joint membrane, capsule, tendon substance, and bursal floor, because they are here welded into one single structure. Nor is there a clear line of demarcation on the proximal side of the short tendon, where the muscle begins.
2. "The Torpedo Cells" are so called from their shape. They are probably merely modified cartilage cells which lie in the palisades with their long axes parallel to the columns. They closely resemble the cells of the adjoining articular cartilage, but their intercellular substance is more fibrous. They seem to function in making the columns, or palisades, and also in forming the blue line.
3. "The Palisades," i.e., the portion of the tendon inserted in the tuberosity, is thus named because of its columnar fibers. In cases of complete rupture of the tendon, the stub, which often remains on the tuberosity, represents this structure. It is fibro-cartilaginous in consistency and contains many "torpedo cells."
4. "The Blue Line." With the hematoxylin and eosin stain there is always, in adults, a blue line (of course, really a surface) where the palisades are inserted into the bone. The blue line is not present in infancy and even in a specimen from a girl of eighteen (Plate VI), it is not well developed; i.e., the cells stain blue, but there is little deposit outside the cells as compared to the amount of blue non-cellular material one finds in older patients. The blue line is very close to the surface of the bone, but appears to be fenestrated for the insertion of the tendon.
5. "The Armor of the Sulcus" is the superficial layer of bone on the facets which we find in the dried specimen, and is really the cortical bone beneath the blue line. Like the trabecule it takes a pink stain. The armor in a normal tuberosity should be almost smooth on its surface; i.e., in section it should give a definite regular outline. It is a surprisingly thin layer considering the stress it must bear; beneath it are marrow spaces and cancellated bone.
6. "The Synovial Reflection" is the angle between the edge of the articular cartilage and the palisades. It is described on pages 15-16, Chapter I, and is illustrated in Figs. 9 and 10. In dissecting room subjects this angle is seldom normal; there is almost always evidence of rupture of some of the columnar fibers of the palisades, as in Fig. 9.
7. "The Finger-like Processes" pass through the blue line, and form a singularly strong attachment to the bone beneath. These processes usually contain cells similar to the torpedo cells but apparently charged with calcium, for when close to the bone they take a deep blue stain.
8. "The Articular Cartilage" definitely begins at the very edge of the sulcus where the tendon is inserted. There is a sharp line between it and the "palisades"; i.e., the synovial reflection.
9. "The Cancellated Bone," or Spongiosa, forms the bulk of the head of the humerus. The spaces usually contain fat and scattered marrow cells, and are not normally very vascular. Both the blue line and the armor are continuous with similar but less pronounced structures, beneath the articular cartilage, where there are no finger-like processes and where there appears to be a cleft between the blue line and the bone under the cartilage.
PLATES III AND IV
The cuts in Plates III and IV are made from direct photographs of some of Dr. Akerson's slides of old lesions found at autopsy. Those on the left are enlarged two diameters, and those on the right about four diameters in each case.
PLATE III
Figure 1 shows a beginning tear of the fibers at the synovial reflection, a little more extensive in degree than that shown in Fig. 9 in Chapter I.
Figure 2 shows a still more extensive rupture of the deep fibers, i.e., a. " rim rent." More than half of the tendon has been torn away, leaving portions of the columnar fibers (palisades) still attached to the tuberosity. The little hook which is in the center of the small circle is all that remains of the former synovial reflection. One small cavern is present in the tuberosity, which also shows evidence of slight excrescences.
Figure 3. A section from the same specimen as that shown in Plate V, Fig. 6, but taken near the edge of the gap, so that there is continuity of some of the superficial portion of the tendon with the external part of the palisades. It would be hard to explain this section or No. 4 by erosion from contact with the acromion process.
Figure 4. Another section from the same specimen which shows a partial rupture in the central portion of the tendon, and yet the fibers are continuous with the palisades, superficial to, and also beneath, the torn fibers. Most specimens show, when sectioned, this same irregularity in the extent of rupture in the different layers of the tendons. Compare the frontispiece, and imagine the degree of tearing in each layer which would be shown by a section at the left of the rupture.
PLATE IV
Figure 1. A very old complete rupture in which recession has taken place; no evidence of either sulcus or tuberosity left; the whole surface of the tuberosity has become rounded off to avoid friction. It is not enough to say by friction. The process of recession is a response to friction rather than a result of it. The fibrous layer which occupies the place of the tendon is not true tendon substance, but a portion of the roof of the bursa, the entire fioor of which has disappeared.
Figure 2. A recessed tuberosity where no sign of sulcus or eminence remains. In the falciform edge of the torn tendon is a small oval speck of bone which formerly was the facet of insertion of the tendon. This is pretty definitely proven, not only by the gross appearance of the specimen, but by the fact that under high magnification one can still see evidence of the blue line on the periphery of the fragment. In this way nature manages to reduce friction even where a fragment of tuberosity is evulsed.
Figure 3. Section through an excrescence which has deformed the armor and the blue line in this region; yet under high power there are none of the usual evidences of inflammation, such as lymphocytes or increased fibrosis of the marrow spaces. The synovial reflection is relatively normal and so are the palisades, internal and external to the excrescence.
Figure 4. A rim rent where all the tendon is torn away from the sulcus except the superficial portion which extends into the periosteum. Partial recession has occurred. Some of the columnar fibers are still present in the deformed sulcus.
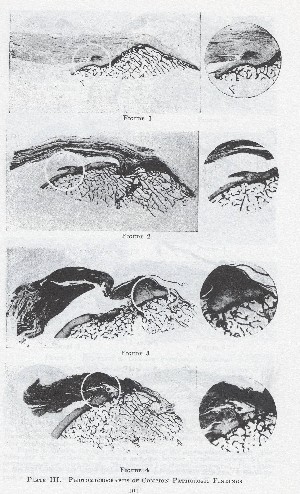
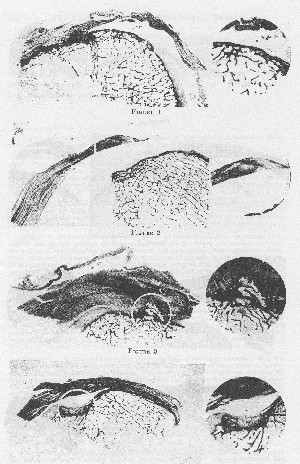
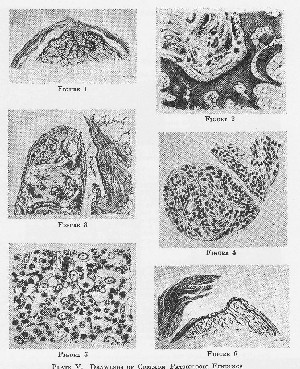
PLATE V. DRAWINGS OF COMMON PATHOLOGIC FINDINGS
Figure 1. Section of the greater tuberosity in an old case of rupture of the supraspinatus. It shows the presence of "caverns" containing vascular tissue. The section is taken through an excrescence or "volcano." A section of the same specimen taken in a more transverse plane shows the caverns as rounded, cystlike spaces.
Figure 2. High power picture of the lower end of one of these caverns, indicating the vascularity of the tissue within.
Figures 3, 4 and 5. Illustrations of a few of the varied appearances presented by villi found in chronic inflammation of the bursa. Fig. 8 shows fibrous, vascular and fatty changes, and Fig. 4 shows richly cellular areas. The section, Fig. 5, showing infiltration with polynuclears was taken from the case reported on page 247. There was no gross evidence of suppuration in this wound, but old silk stitches were causing irritation of the tissues.
Figure 6. Section through an old rupture of the supraspinatus tendon. The tuberosity is in process of recession and has become atrophied except for an excrescence at the outer margin. The blue line has almost disappeared. The armor is lacking because for years there has been no functional stimulus. Eventually such a tuberosity would become almost completely rounded off.
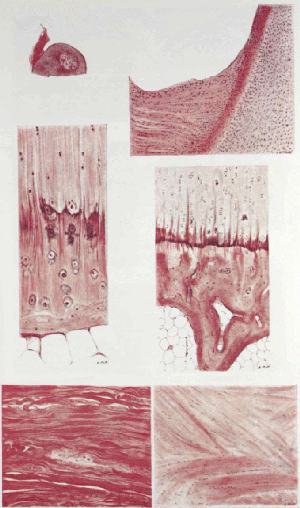
PLATE VI. HISTOLOGY OF TENDINOUS INSERTIONS
PLATE VI
1. Section .through the attachment of the supraspinatus tendon of an infant. The center of ossification of the articular head is present, but those for the tuberosities have not yet appeared. The tendon takes a bright pink stain, while the cartilage, which is to form both the articular surface and the tuberosity, is purple.
2. Higher magnification of the "synovial reflection" in the same specimen. It shows the line which separates the tendon from the cartilage which is later to form the tuberosity. The coloration of the intercellular substance (i.e., the acidity or alkalinity of the tissue), rather than the morphology of the cells, is the distinguishing feature. Sections of this region from children up to at least the age of twelve show no very definite blue line of demarcation between these two structures, but in sections from a girl of eighteen (Fig. 3) there is the suggestion that the blue line is in process of formation. It therefore probably begins to form somewhere between twelve and eighteen.
3. Section through the cortical (armor) bone of the tuberosities in a girl of eighteen. In this section the blue material appears to be chiefly in and about the cells (bone corpuscles?) in the armor. It suggests that these cells are instrumental in causing the blue deposit. They appear to leave it behind as a kind of shellac for the finished adult surface of the armor of the tuberosity. Whether they die when they have finished this work or whether they leave the deposit behind and proceed upward to become fibrocartilage "torpedo cells" is a matter for histologic research. The present theory is that they do not proceed up into the tendon. In this young girl, the bone below the blue line is rich in cells, but in adult life (Fig. 4) there are relatively few living torpedo cells in the armor. Dr. Wolbach tells me that the formation >of this blue line resembles to some extent histologically the formation of enamel in a tooth.
4. This section shows what is usually found in an adult specimen. The blue line appears to be entirely extracellular and the fibrocartilage cells, which I have called "torpedo cells," in the palisades are very conspicuous. There often occur little masses of purple, crystalline collections, as indicated in this picture, just above the blue line. They are sometimes found even further up in the palisades. Their appearance suggests that they may be somewhat abnormal deposits, due to the failure of the cells to leave their blue staining material in the region of the surface of the bone. It is possible that a knowledge of their formation would throw light on the formation of the peculiar calcified deposits which occur in the tendon at a higher level. In both Figures 3 and 4, notice the finger-like processes which pass down (or it may be pass up?) through foramina in the blue line. Evulsion of these fibers may occur or a portion of the blue line may be retracted with the tendon.
5. A section taken from the supposedly normal adult tendon shown in Figure 9. On study with high power it shows deeply staining areas in the tendon substance which give evidence of abnormality of the collagen. It also shows abnormal changes in the torpedo cells.
6. Early changes in the character of the collagen of the fibrocartilage which composes the palisades. When the collagen is in this condition, the degenerative portions may be indicated by either a bluish or a pinkish stain with H and E.
We may now briefly take up the changes which are often found in these structures.
1. The critical portion of the tendon may show many shades of stain according to the degree of necrosis. It may contain large calcified areas or minute specks or merely necrosed fibers without any deposit. It may show rupture of all the fibers or of only those of the central or peripheral parts.
2. The torpedo cells undergo very interesting alterations. They may become calcified or enlarged into peculiar giant cells, or they may fade.
3. The palisades often show irregular staining qualities indicating necrotic changes; broken fibers, rice bodies, etc.
4. The blue line is a curious structure which is present at most points in the body where cartilage or tendon is attached to bone. It may become irregular on its surface or embossed by the formation of bony excrescences beneath it. It may be torn out in patches by the tendons.
5. The armor may become greatly thickened (eburnated) in laboring men from excessive use of the tendon. It may also become thickened from chronic inflammation in the tendon. Where the blue line is destroyed, the armor is thin; e.g., after recession of the tuberosity it is usually quite thin, and the blue line has disappeared.
6. The synovial reflection is almost always changed to some degree as rim rents form. In most elderly patients we find at the angle of reflection that the columns of the palisades are more or less torn.
7. The finger-like processes may also show evidences of necrotic changes if staining reactions may be considered evidence. I strongly suspect that increase of the calcium deposits in the blue line may choke off these fibers so that the tendons may be more easily pulled out.
8. The articular cartilage may show thinning and superficial loss of substance but usually appears unchanged even to the very edge.
9. Vascular caverns may be formed in the spongiosa near the facets.
There are many other interesting and suggestive points about the pathologic histology of these lesions, but the above-mentioned changes may be readily confirmed by any one who has access to autopsy material. This is an uncultivated pathologic field except for Dr. Aker-son's work. Correct interpretation of the common findings is greatly needed so that our clinical results may be improved. To my mind one of the most promising leads for the pathologist is that concerned with the extreme sensitiveness which the tendons show to hematoxylin and eosin stains. Sometimes the necrotic portions are pink or red, and sometimes blue or purple. Notice the staining of the section from the infant's humerus. Why should the contrast be so pronounced? In the adult why is the bone red and the blue line blue? What phases of necrosis attract the blue or the red stain? Could these tissues be acidified by either local or general use of drugs? Could the pathologic process in tendinitis be checked by increasing or diminishing the acidity of the blood or in any way by altering its constituents ?
REFERENCES
CODMAN-, E. A., AND AKERSOH, I. B., The Pathology Associated with Rupture of the Supraspinatus Tendon, Annals of Surgery, Phila., 1931.
GHUBER, W., Hygrom der Bursa mucosa subacromialis, Oesterr. Z. f. prakt. Heilk., Wien, 1869, xv, 819; Also: Ein Hygroma retroglenoidale scapula?, Arch. f. path. Anat., etc., Berlin, 1875, lxv, 288-241.
MOSCHCOWITZ, E., Histopathology of calcification of the spinatus tendons, as associated with subacromial bursitis, Proc. N. Y. Path. Soc, 1915, n.s., xv, 1-7; Also: Am. J. M. Sc, Phila., 1915, cl, 115-126.
SCHWABZ, E., Untersuchungen tiber die Entstehung der Zotten und Reiskorper in Hygromen sowie die sogenannte "fibrinoide Entartung" des Bindegewebes der Schleimbeutelwand, Dtsch. Z. f. Chir., 1931, ccxxxv, 1-3; Also: Dtsch. Z. f. Chir., 1982, ccxxxv, 140-163. (Contains some excellent photomicrographs of the so-called rice-bodies which are often found in bursa? and which are demonstrated again and again in Dr. Akerson's collection; references are given to most of the important articles on the pathology of bursa; in general, but there is no mention of the subacromial bursa.)
STIEDA, A., Zur Pathologie der Schultergelenkschleimbeutel, Arch. f. Klin. Chir., Berlin, 1908, lxxxv, 910; Also with BERGEMANN, Ueber die mit Kalkablagerung einhergehende Entziindung der Schulterschleimbeutel, MUnchen med. Wchn-schr., 1908, lv, 2699-2702.
Brief references to the pathology of this region are also made in some of the papers listed at the end of Chapter VI.


